Box Turtle Bulletin
 News and commentary about the anti-gay lobby
News and commentary about the anti-gay lobby News and commentary about the anti-gay lobby
News and commentary about the anti-gay lobbyPosts Tagged As: Health
November 25th, 2015
As I have discussed in a series of articles, obtaining pre-exposure prophylaxis (PrEP) for HIV is not simply a matter of asking your physician. Depending on your health insurance, it may be extremely difficult to get a prescription for Truvada, the medication that with proper use prevents HIV infection. For example, for the 10 million residents of Los Angeles County, there is only one clinic that provides PrEP and accepts Blue Shield HMO coverage.
It would appear that this scarcity is not limited to Los Angeles, and this concerns the Centers for Disease Control. (http://www.cdc.gov/nchhstp/newsroom/2015/vital-signs-prep-press-release.html)
“PrEP isn’t reaching many people who could benefit from it, and many providers remain unaware of its promise,” said CDC Director Tom Frieden, M.D., M.P.H. “With about 40,000 HIV infections newly diagnosed each year in the U.S., we need to use all available prevention strategies.”
…
“PrEP has the potential to dramatically reduce new HIV infections in the nation,” says Jonathan Mermin, M.D., M.P.H, director of CDC’s National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention. “However, PrEP only works if patients know about it, have access to it, and take it as prescribed.”
The CDC is now recommending that about 25% of gay men take PrEP, based on a number of criteria. It has awarded about $216 million to organizations that are targeting at risk communities.
November 20th, 2015
 After several weeks of effort, I was able to find a doctor within the Blue Shield HMO plan who prescribes Truvada as Pre-Exposure Prophylaxis, PrEP. The source of my primary care is now through APLA Health and Wellness at the Gleicher / Chen Health Center in Baldwin Hills.
After several weeks of effort, I was able to find a doctor within the Blue Shield HMO plan who prescribes Truvada as Pre-Exposure Prophylaxis, PrEP. The source of my primary care is now through APLA Health and Wellness at the Gleicher / Chen Health Center in Baldwin Hills.
This feels a bit ironic to me. For years I’ve sporadically supported AIDS Project Los Angeles. I’ve participated in the AIDS Walk from time to time and contributed to various programs but they weren’t particularly applicable to my life. They were just a “good organization” with whom I didn’t much interact.
Thursday evening was my first appointment. There was almost no one in the waiting room and the staff was more than pleasant. The employees seemed to be genuinely enjoying their work and their interaction with patients. The office, which is only a year old, was spotless, well lighted, and comfortable.
I didn’t see my doctor yesterday.
Before Truvada is prescribed, a series of tests needs to be run. There was blood work taken for two HIV tests (one which identifies more recent exposure), a liver test, as well as the usual lab work. Urine and swab samples were taken to indentify any sexually transmitted infections. And, of course, there were questions about recent sexual history and practices.
The nurse-practitioner was friendly, informative, and willing to answer questions. She was aware that some personal questions are uncomfortable and made the process feel professional rather than invasive.
We discussed the changes in care and protection over the years and the hopes for the future. Although we both celebrated the changes we’ve seen, she expressed concern about how a younger generation sees HIV like it sees diabetes, not terribly serious. A long time AIDS care provider and community advocate who has lost many friends to the disease, she’s disappointed that more people are not availing themselves of PrEP. I share that feeling.
But now I wait.
In two weeks I will return for my results and, if everything is proper, I’ll get my prescription and join the ranks of those who are proactively protecting themselves from the HIV virus.
November 10th, 2015
 In my last update, I reported that Blue Shield HMO had provided me with the name of five doctors who they thought do prep. So I’ve made some phone calls.
In my last update, I reported that Blue Shield HMO had provided me with the name of five doctors who they thought do prep. So I’ve made some phone calls.
First I eliminated the doctor who practices in Santa Paula, 70 miles away in another county. That’s a bit too far to drive every three months during office hours and I certainly wouldn’t want a primary physician that far away.
Then I called the doctor who doesn’t do PrEP at all; he only does HIV testing. Which I do myself using OraQuick, the at-home testing kit.
Next was the doctor who does do PrEP, but not through my insurance. He only accepts patients with my insurance if they are already HIV positive.
Finally, I called the last number (the two remaining doctors practice together). I was transferred to a voice message of someone who I believe said that he is the PrEP coordinator for APLA.
So there is still some hope that this final contact will come through and I will finally have access to the program.
UPDATED
I heard back from the PrEP coordinator and it turns out that the doctor does take my insurance, administers PrEP, and is accepting new patients. He’s 6 miles away and only about a half-hour drive, so I’ve changed my primary care doctor and have an appointment for next week.
This has not been an easy process. But it has proven to be possible, something I was not sure about for a while.
November 7th, 2015
 On Thursday I shared with you the surprising difficulty of finding a doctor within my health network that will prescribe pre-exposure prophylaxis (PrEP), a proactive approach to avoiding HIV infection.
On Thursday I shared with you the surprising difficulty of finding a doctor within my health network that will prescribe pre-exposure prophylaxis (PrEP), a proactive approach to avoiding HIV infection.
Since then I’ve received help and suggestion from several sources, including in the comments here at BTB. Thank you.
I dropped by the new West Hollywood outpost of the Los Angeles LGBT Center and, though it was after hours, the young man at the desk sought to be helpful. I’m not sure that I was able to adequately explain that I needed to know whether they would honor my insurance or that I needed to find a primary care physician, but he did provide me with the main number of the Center.
I also had a response from a pharmacist who was able to recommend two sources: the LGBT Center, which he warns has a two month waiting list, and an HIV treatment center 25 miles away. Neither of these options seem ideal.
But yesterday I did hear back from Blue Shield. And they were able to provide me with a comprehensive list of all of the doctors in the network who offer PrEP service in the Los Angeles area. There are a grand total of five.
Now I need to see if any of them are willing to add a new patient.
November 5th, 2015
 Today Larry Kramer, the grandfather of ACT-UP, released a scathing indictment of the current status of AIDS research. And though he was in parts incoherent (gonorrhea statistics don’t speak to AIDS research funding), his frustration has merit. Bureaucratic structures don’t lend themselves well to efficiency and as decades slip by with the oft-promised cure remaining just out of sight, it becomes easy to agree that the National Institutes of Health are “more interested in Alzheimer’s than AIDS and Congress is not interested in AIDS at all”.
Today Larry Kramer, the grandfather of ACT-UP, released a scathing indictment of the current status of AIDS research. And though he was in parts incoherent (gonorrhea statistics don’t speak to AIDS research funding), his frustration has merit. Bureaucratic structures don’t lend themselves well to efficiency and as decades slip by with the oft-promised cure remaining just out of sight, it becomes easy to agree that the National Institutes of Health are “more interested in Alzheimer’s than AIDS and Congress is not interested in AIDS at all”.
Kramer is the king of rage. His anger has propelled a life-long fight against institutional power, even as Kramer has gained access to levels that most of us could never achieve. And though many of his demands over the years have been met, his bleak view has never been at loss for a target of his fury.
But, frankly, a life lived in outrage is exhausting. And my temperament doesn’t allow me to see the world through the prism of loss and lack.
Like Kramer, I lived through the years of fear and frustration in the 80’s and 90’s and have lost friends to AIDS, though likely not on the same scale. And I too have seen Very Exciting Breakthroughs For A Cure that turned out to be anomalies and overblown wishes. I now approach each new cure-around-the-corner claim with the skepticism of the man who discovers that he did not, after all, buy the Brooklyn Bridge.
But I have experienced the arc of the epidemic. I recall when nothing was known about Gay-Related Immune Deficiency (as it was first called) and then when the Human Immunodeficiency Virus was identified. I know the growing panic during the two-week response period. I remember the breakthrough of the mid-90’s when the “drug cocktail” of antiretroviral treatment caused the death rate to plummet. And since then I’ve watched a plodding but steady progression towards management and sustainability and prevention.
There has been amazing progress.
Yes, HIV continues to impede the full potential of lives. Even in the best of cases, it brings a tedious drug regimen, social stigma, and the fear of unknown possible side effects.
But unlike Kramer, I just can’t see the glass as half full and draining rapidly. Irrespective of whether the NIH appoints a new head of the Office of AIDS Research in a timely manner, I still see the glass as three quarters full with a steady drip increasing the level.
And one of the more recent developments that has given me hope that the viral endemic can finally be beaten has been the two pronged approach of undetectability and insusceptibility.
For most (but not all) HIV infected persons, current drug treatments reduce the level of virus in the body to such a point that it cannot be detected. And the practical reality is (though officials are hesitant to stake this claim) those with undetectable levels of HIV are not transmitting the virus to others.
And more recently, within the past couple of years, it has become evident that pre-exposure prophylaxis (PrEP) in the form of a daily dose of Truvada can cause an HIV negative person to be virtually immune from contracting the virus. By virtually immune, I mean percentages in the high 90’s, a better success rate than condoms. Though anecdotes do not speak definitively, at this point the collective street-knowledge of PrEP is nothing short of astonishing. As a small example, an acquaintance of mine who is seriously dedicated to condomless receptive anal sex and who was one of the early participants in PrEP tested negative again yesterday after a couple years of regular “unsafe” sexual practice.
In combination, these two therapies may not be the cure that Larry Kramer and the rest of us hope for, but if correctly targeted and implemented, we could see HIV in America go the way of tuberculosis in a generation.
Of course, that requires thoughtful and committed leadership. And I do have skepticism about the commitment of government to properly design or implement such a plan.
I suppose it’s possible that a driven and charismatic leader will be appointed to the Office of AIDS Research who will throw political expediency out the window and press towards targeting the communities that most need regular and thorough testing and who is willing to buck powerful elements of the AIDS industry who have a vested interest in opposing PrEP. I suppose someone could don a cape and come to our rescue.
But the history of the AID epidemic suggests otherwise. For the most part, power and government have impeded rather than advanced response. It has been mostly gay men, and their allies (let’s never forget how lesbians stepped up to a crisis to which they are least directly threatened) who have been on the forefront of knowledge and power, who played personal guinea pig, who recrafted the social acceptability of practices within their own community, and who fought in the streets for the right to take drugs that would save their lives.
So I suspect it will be up to the gay community to create a culture in which all of those who HIV positive are tested and place on appropriate medication (and fight for the funding to make this a reality) and all those who are sexually active outside of a monogamous relationship and who are negative go on PrEP (a likely tougher funding fight). We will have to be the ones who make “Truvada whore” a badge of responsibility and sexual freedom.
Yes, we will need to be conscious of possible side-effects and aware that all drugs impact different bodies differently. But – at least so far – it appears that until a cure for AIDS is discovered, PrEP is a promising approach to personal protection and community health.
So it’s time to do my part. It’s time for me to join the Truvada whores, time to take PrEP.
Over the past months, several of my friends have gone to their doctors and signed up. They are all happy with this choice and found it to be a painless process. I’m not so lucky.
My employer provides me with health insurance through Blue Shield of California (for which I am appreciative). My plan is an HMO and though that is more limiting than a PPO, it hasn’t really impacted me much. Until now, I have no complaints. Or, not many.
When the plan was implemented, Blue Shield assigned me to a primary care physician based on location. And as I live near Koreatown, my doctor operates out of an office which caters primarily to older Koreans.
I’m not Korean, but the diplomas were from reputable schools and as my medical history is not complex, I figured that any doctor can provide basic care and I had no reason to change. And, frankly, it felt a bit prejudiced to discount a doctor’s ability to treat me simply because I’m not in his target demographic.
And for the most part, all has been fine.
Yes, there was the time he pressured me to become vegetarian (ummmm, no!). And, as I discovered in the waiting room, I’m not a big fan of Korean soap operas. But he was attentive and personable and I just don’t see a doctor that much.
On my last visit, I told my doctor that I was interested in PrEP. He had no idea what I was talking about so I asked him to look into the subject so that we could pursue that direction. He said nothing.
Finally, having waited for months without a response, I called my doctor’s office and explained to the receptionist that I’d like to see the doctor and would like to discuss PrEP with him and could he please be ready for this. She said she’d ask the doctor.
The receptionist called me back. And said I should find another doctor. One that deals with HIV. Because my primary care physician wouldn’t want to give inadequate care.
It’s probably only my imagination that heard “go away, go away, don’t touch me”.
But fair enough. I’m certain that his knowledge of his community allows him to be aware of cultural particularities which give him greater insight into the care of his specific demographic. And I probably would be better served by finding a doctor who is familiar with the trends in the lives of gay men and specific medical issues of which to be aware.
Besides, I live in Los Angeles. There are more than 25,000 doctors in this county. How hard can it be to find one that specializes in gay health (or “men’s health” as it is sometime euphemistically called)?
As it turns out, it’s not so easy.
My insurer’s website easily allows you to search for another primary care physician. You can search by gender, language spoken, medical specialty, or name. You can even put in other search terms. But gay and LGBT had zero results.
So I turned to Yelp. Here, results were more promising. Several reviews discussed whether the doctors were welcoming of gay men and women. Some even discussed PrEP. Best of all, Yelp’s ad generator gave me the names of medical groups who specialize not just on gay men but on getting them onto PrEP. Yay!
Back to the website I went. The most prominent men’s health group didn’t show up. But fine, another did. So I submitted my change request and waited.
Nothing.
So back to the website I went and sure enough, my primary health group is still the Korean group.
This time I didn’t rely on the doctor’s name showing up in the grid to mean that I could select that doctor. I called or emailed the doctors instead. And it turns out that none of them accept Blue Shield HMO. Zero success.
Back to online searching. Viola, there are handy guides to tell one just who does administer PrEP in LA County. But sadly, they seem to either be upscale and take PPO or other high end insurance plans or else they cater to those less fortunate and take Medicare. For someone who has (what I’ve assumed to be) a perfectly fine but no frills plan, there seems to be nothing.
In desperation, last night I called Blue Shield. And the lovely young women who handled my call agreed to search their database for doctors in LA who take my insurance plan and who specialize in PrEP (who knew it had to be a specialty?). After 20 minutes holding, she came back to tell me that she had no success. But she promised to keep trying and to call doctors until she found me one.
However, I’m not over-confident of hearing back. Because when I suggested that she broaden her search to include gay health or men’s health she became flustered and confused. I’m guessing that in whatever culture she live, one doesn’t say the words “I’m a gay man” out loud.
But I’m not giving up. I do have some leads.
One of the doctor’s offices – one that doesn’t take my plan – generously came up with some names of others who might be able to direct me. And the local LBGT center is a resource that I can approach. Word is that they’ve opened a new outreach office in West Hollywood whose sole purpose is to get gay men on PrEP and I’m hopeful that they might be able to help.
I am confident that eventually I’ll find a doctor that takes my insurance plan who is willing to provide this regimen. I live in a city that is, for the most part, inclusive and welcoming of gay people. I have many many options and opportunities.
But I cannot imagine trying to go through this process in a red state. Or in rural California. Or in a city without an established gay community.
So maybe Larry Kramer has a point. PrEP should be available to every gay man – or every other person in a high risk demographic – through every doctor in the country, not just the handful who “specialize” in gay health. We would not find it acceptable if this level of difficulty were faced by those who sought preventative measures for anything else? Why is it acceptable that doctors can turn away patients simply because they “don’t deal with HIV issues”?
Maybe Kramer’s right. Maybe it is time for a little rage.
December 19th, 2011
Maggie Gallagher, the nation’s chief opponent to marriage equality, loves to claim that marriage is good for society because those who are married live healthier lives. And a new study appears to confirm that claim.
From the NY Daily News
A report published in the American Journal of Public Health shows that in states where gay marriage is legal, homosexual men visit doctors less and their health costs go down considerably.
“Our results suggest that removing these barriers improves the health of gay and bisexual men,” Mark Hatzenbuehler, a Robert Wood Johnson Foundation Health & Society Scholar at Columbia University’s Mailman School of Public Health, said in a news release
Of course, Maggie only meant heterosexuals who are married. Alas.
I didn’t really need a study to know that those who are in committed relationships take fewer risks, enjoy greater contentment, and have someone there to nag them about their weight. But it’s nice to have confirmation… Of sorts.
To be honest, I don’t place much faith in this actual study. Comparing one year to another year in one clinic has about as much statistical value as guessing. But I guess it did at least show that enacting equality doesn’t lead to increased health costs – as The Peter absurdly likes to imply.
But Maggie and her NOM buddies just love statistically irrelevant studies and if she were consistent she’d see this as evidence in favor of marriage equality.
So does that mean Maggie will switch sides and support marriage? Nope. Even if this were irrefutable proof that marriage equality would improve the health of ever gay person with no negative consequences for anyone gay or straight, Maggie would still fight to keep inequality in place. Because your health is a far far lower priority than having her church get to dictate what law and culture should allow.
January 28th, 2011
“Defenders of traditional marriage” like to pretend that their objections to marriage equality are based in procreation or what’s best for children or religious freedom or culture or something, anything, other that bias, animus, or a desire to harm gay people. But sometimes their real motivates leak through the front they present to the world.
Take, for example, this portion of an essay by the National Organization for Marriage’s Maggie Gallagher:
Anal sex is painful, unsanitary, unsatisfying for women, and creates unique risks for serious physical diseases (if you doubt me, go read the Wikipedia entry on the subject) because the anus is not designed for sexual intercourse, increasing the risk of torn flesh and the intermingling of bodily fluids — blood, semen, fecal matter — that can spread an astonishing variety of diseases. The female partner is far more at risk than the man in these encounters. This should be a feminist issue.
Now, of course, Maggie is directing this rant to women. So it has nothing, no nothing at all, nope not whatsoever, to do with her views about homosexuality. And as some gay men don’t engage in anal sex and few lesbians as well, well then obviously this say nothing, no nothing at all, about Maggie’s perspectives of gay people in general. Right?
Except that Maggie isn’t just condemning heterosexual anal sex. In fact, that isn’t her target at all.
In the minds of anti-gay activists and others to whom Maggie directs her essays, homosexuality is inextricably linked with anal sex (lesbians exist as an after-thought). When a preacher rants, “it’s not natural,” and you know he’s thinking anal sex. Hear a politician declare, “that’s not how the body was created,” and it’s anal sex he’s discussion. See an erudite talking head with crisply parted hair and wire-frame glasses espousing his views on “complimentarity” and guess what he means? Anal sex.
So when Maggie attacks anal sex with imagery of “torn flesh” and blood and fecal matter and “astonishing variety of diseases,” it really isn’t about young women at all. Sure, she’d rather they engage only in vaginal intercourse with their lawfully married husband, but that isn’t her point. Rather, Maggie sees this as “dirty” and “icky” and, let’s be real, a homosexual practice that godly heterosexuals should have nothing to do with.
Maggie is generally pretty good at hiding her personal contempt for gay people. But sometimes, like this time, it seeps around the edges.
July 1st, 2010
 The gay health insurance tax is such an odd, unfair, and blatantly discriminatory tax that many heterosexuals have difficulty understanding it – or even believing that it exists. Here’s how it works:
The gay health insurance tax is such an odd, unfair, and blatantly discriminatory tax that many heterosexuals have difficulty understanding it – or even believing that it exists. Here’s how it works:
Suppose Joe and Susan are married. Joe has a job with great benefits and Susan works part time as a freelance artist so they take advantage of Joe’s health plan to cover Susan and their two children. The company pays the premiums and everyone is happy.
But if Joe is Janet, the rules change. Janet works at a great company which does not discriminate between gay and straight couples. It recognizes her marriage to Susan and provides health coverage to Susan and their two children just as it would if Janet were Joe.
But now the federal government pops its head in to object. For tax purposes, family benefits are not considered part of your taxable income. Unless you are a same sex family, in which case the federal government says that you are not a family at all. If you are a same-sex couple then you have to pay the Gay Health Insurance Tax.
“Susan is not a relative,” they say. “She’s just some random stranger who is being covered by your health plan. And these kids are her children, not yours.” So, as Susan is not Janet’s spouse according to federal law, they do not treat the health insurance premiums which cover Susan and the kids as family benefits.
“This is income,” they say. Just as any other amount taken from your check and paid to a third party (say a creditor with a lien) is considered part of your income, so too are these insurance premiums paid to cover this other random non-spouse person considered part of your income.
And so they tax Janet. Assuming that Janet is in the 35% tax bracket, her wonderful company may give her coverage for Susan for which they pay premiums of $500 per month, but the IRS gives her a tax bill for $175. So while Joe and Janet may do the same exact work and receive the same exact pay, Joe takes home an extra $2,100 per year.
Now some companies are seeing this as unfair. They support the idea of equal pay for equal work and are stepping in to make up the difference. The latest (and largest) is Google. (NY Times)
On Thursday, Google is going to begin covering a cost that gay and lesbian employees must pay when their partners receive domestic partner health benefits, largely to compensate them for an extra tax that heterosexual married couples do not pay. The increase will be retroactive to the beginning of the year.
This is great news for Google’s gay workforce. But it is also good news for those who work at other companies, especially those with whom Google competes for skilled high tech employees.
But given the competitive nature of the benefits culture in Silicon Valley, where companies often offer extra perks to attract top employees, Google’s decision could lead to policy reviews, experts said.
“It could have a ripple effect, prompting other employers, and particularly employers in the same industry, to take a look at their own benefits package and see whether it would be appropriate to extend those benefits,” said Kathleen Murray, principal in the health and benefits consulting business in San Francisco for Mercer, the consulting firm. “When you have a high-profile company doing anything, that tends to get into the mind of the culture, and it can have a more diffuse effect.”
And as more companies begin to recognize the special gay health insurance tax levied specifically at gay couples, the more the public becomes aware of this bizarre inequality and the easier it becomes to get it changed. A provision which would eliminate the tax was at one point part of the health care reform but did not make it to the final bill.
It seems that some of our representatives believe that gay people should pay higher taxes than heterosexuals. Ironically, they are the ones that you often hear calling for tax cuts… just not for us.
April 5th, 2010
From the Kansas City Star
increasingly accurate tests have been developed to detect HIV in donor blood. The first tests that became available spot antibodies that the immune system produces when confronted by HIV. It usually takes two to eight weeks, but sometimes longer, for the body to make enough antibodies for the tests to detect.
A newer test can find HIV itself in the blood. This test shortens the time between infection with the virus and detection to nine to 11 days.
March 13th, 2010
From the LA Times:
Federal health officials announced Friday that they would reexamine a 27-year-old set of restrictions on blood donations by gay men.
…
The FDA “has been actively engaged in reexamining the issue of blood donor deferral for men who have had sex with other men, taking into account the current body of scientific information, and we are considering the possibility of pursuing alternative strategies that maintain blood safety,” the agency said in a statement.The issue will be examined by the Department of Health and Human Services’ blood safety committee in June, according to the statement.
This commentary is the opinion of the author and does not necessarily reflect that of other authors at Box Turtle Bulletin.
March 8th, 2010
 In 1983, the FDA established a policy requiring that blood banks not accept donations from any male who had engaged in sex with any other man at any point since 1977. This was implemented so as to attempt to eliminate blood which was potentially infected with the HIV virus from the pool, and it made sense at that time.
In 1983, the FDA established a policy requiring that blood banks not accept donations from any male who had engaged in sex with any other man at any point since 1977. This was implemented so as to attempt to eliminate blood which was potentially infected with the HIV virus from the pool, and it made sense at that time.
It wasn’t until 1983 that the HIV virus was identified, and a method of testing for the virus wasn’t established for another two years.
In 2006, the AABB, America’s Blood Centers, and American Red Cross jointly asked the FDA to reconsider these rules. They argued that continuing the ban was not justified by scientific advances since the ban was implemented.
AABB, ABC and ARC believe that the current lifetime deferral for men who have had sex with other men is medically and scientifically unwarranted and recommend that deferral criteria be modified and made comparable with criteria for other groups at increased risk for sexual transmission of transfusion-transmitted infections. Presenting blood donors judged to be at risk of exposure via heterosexual routes are deferred for one year while men who have had sex with another man even once since 1977 are permanently deferred.
Current duplicate testing using NAT and serologic methods allow detection of HIV- infected donors between 10 and 21 days after exposure. Beyond this window period, there is no valid scientific reason to differentiate between individuals infected a few months or many years previously. The FDA-sanctioned Uniform Donor History Questionnaire was developed recognizing the importance of stimulating recall of recent events to maximize the identification of donors at risk for incident, that is, recent, infections. From the perspective of eliciting an appropriate risk history for exposure to HIV and other sexually transmitted infections, the critical period is the three weeks immediately preceding donation since false negative NAT and serology reflect these window-period infections, and the length of these window periods provide the scientific basis for the deferral periods imposed for at risk sexual behaviors.
The FDA refused.
They argue that as gay men have a higher concentration of HIV infection than some other demographics, this justifies a blanket ban on all donations by all gay men.
Men who have had sex with men since 1977 have an HIV prevalence (the total number of cases of a disease that are present in a population at a specific point in time) 60 times higher than the general population, 800 times higher than first time blood donors and 8000 times higher than repeat blood donors (American Red Cross). Even taking into account that 75% of HIV infected men who have sex with men already know they are HIV positive and would be unlikely to donate blood, the HIV prevalence in potential donors with history of male sex with males is 200 times higher than first time blood donors and 2000 times higher than repeat blood donors.
This week, Senator John Kerry, along with several other Senators, sent a letter to the FDA requesting that they reconsider their rules.
“Not a single piece of scientific evidence supports the ban,” the Democratic senator said in a statement. “A law that was once considered medically justified is today simply outdated and needs to end, just as last year we ended the travel ban against those with HIV.”
I doubt that this will be effective. If the FDA refuses to listen to those who know the very most about donation, testing, infection, and the blood supply, why would they listen to John Kerry?
But Kerry’s action does allow us as a nation to re-question why the ban is in place. Is it a matter of heath science or a matter of mistrusting (or disliking) gay men?
The FDA argues that any increased risk of tainting the supply is unacceptable. And that allowing gay men to contribute would unquestionably increase that risk.
But is that true? Does the ban effectively increase the safety of our blood supply? Or does it actually do harm?
To answer these questions, I think we need to look closer at the ban and how it functions.
1. The ban is only as effective as it is perceived to be reasonable. Remember, the ban is voluntary; by that, I mean that the only thing which stops donation is a questionnaire and the donor’s decision to answer honestly. If a gay man is determined to donate, he will only be persuaded not to donate if he believes that the criteria of exclusion is based on reason and not on bias.
2. We must assume that only a psychopath would choose to purposefully donate HIV infected blood. And no questionnaire is going to stop a psychopath. Therefore, this purpose of the questions is to eliminate those who are unknowingly infected.
But who donates blood? According to the Red Cross, only 3 out of 100 of Americans donate. And this 3% is not representative of the population as a whole.
Yes, blood donors come from all races, ages, political affiliations, and economic situations. But they have one thing in common, they are motivated by altruism or a belief that it is in the common good that they donate. They donate because it is the “right thing to do”.
And let’s be practical here for a moment. The type of person who donates blood is not generally the type of person who is irresponsible. If you are a ‘give blood’ type of gay man, you are probably also a ‘get tested’ type of gay man.
So the only unaware HIV-positive infected gay men who are likely to be prevented from donating are those who have good reason to believe (falsely) that they are HIV-negative. That’s not a very big demographic.
3. The FDA does not exclude other demographics who are infected at higher rates than the population at large. For example, over half of all new HIV infections detected in 2007 were in African Americans. While many of those infected are also MSM (men who have sex with men, a term used by the infectious disease community), many are heterosexual. Over 60% of women with AIDS are black. (AVERT)
The estimated lifetime risk of becoming infected with HIV is 1 in 16 for black males, and 1 in 30 for black females, a far higher risk than for white males (1 in 104) and white females (1 in 588).
There are many reasons for this (and for godsake let’s allocate more resources to stemming this trend) and I’m not trying to make comparisons or demonize anyone. But it does demonstrate that the FDA’s banning policies seem inconsistent.
The screening does seek to eliminate those women who might have had sex with a MSM or intravenous drug user in the recent past, but it does not issue a blanket ban based on race (nor should it). However, the “ever had sex at any time in your friggin’ life” definition effectively serves as a ban based on orientation.
So while the FDA does not say that the President of the United States is banned from blood donation based on his ethnicity, it does prohibit donation by Rep. Barney Frank.
4. Not all gay men are equally at risk. Homosexual activity does not create HIV. It is a virus, not a consequence of specific sexual acts. Only about 12% of gay men are infected with the HIV virus.
Yet the FDA treats my friends, a couple in their 40’s who met in high school and have been together ever since, the same as it does some gay man who is single and has an active and diverse sex life. Ironically (and amusingly) it considers ex-gays like Alan Chambers to be no less of a risk than the man whose fetish is to be the recipient in unprotected anal sex.
The FDA clumps gay men into a single demographic and assumes that all gay men are at a higher risk than all heterosexuals.
While statistics indicate a rising infection rate among young heterosexual women, their overall rate of HIV infection remains much lower than in men who have sex with other men.
But clumping in this manner is a foolish and rash policy. Contamination is more likely to come from a young single heterosexual woman who relies on the pill than it is from a gay man in a committed relationship who uses condoms regularly.
5. While the ban on gay men donating does not – in my opinion, as discussed in the points above – serve to diminish much risk of contaminating the blood supply with the HIV virus, it is quite effective at something else: labeling all gay people as dirty and diseased.
This universal ban says, in effect, that all gay men are suspect, a cause of concern, human rats carrying contagion. It feeds the myth that gay equals AIDS and lends credence to the anti-gay activists who market in fear and animus.
But is lifting the ban the answer?
I would argue that a full lifting of the ban is not a wise decision. That would increase – at least in some tiny measure – the risk of taint to the blood pool. Rather, I would advise to change the policy in a way that not only increases the blood supply and to reduces stigma but which also could serve an additional medical function.
Obviously the screening questions need to eliminate the risk of undetected recent infections. But such risks should be based on actual behavior based risk, not on stereotyping of communities. This may even serve to reduce the risk of accidental taint from gay men who ignore the current policy as being nothing more than bias.
Science-based periods of either long-term monogamy or sexual abstinence would likely be respected as reasonable and appropriate. Few gay men would argue that every gay man, regardless of sexual history or responsibility, should donate blood.
And revising the rules for donation to match the requests of the Red Cross would certainly be better than the current policy. But I recommend a different approach.
I recommend that all persons who have any risk of HIV transmission – be they gay men, single heterosexuals, or anyone else who could be at risk – be required to take an HIV test as a step in the donation process. Those persons who tested negative and who had no sexual contact for the previous six months (or whatever restrictions are reasonable) could be treated as acceptable donors. The oral swab tests are non-intrusive, give a response in 20 minutes, and are more than 99% accurate.
The current controls over the blood supply do an amazing job at detecting and removing infected blood. But implementing a screening method that is based on measurability rather than voluntary deferral would effectively eliminate unknown carriers, gay or otherwise.
And it would also reach a population of potentially at-risk citizens who might otherwise go undetected.
The single largest contributor to the spread of HIV is unknown infection. Granted, as I discussed above, those gay men who are most likely to donate blood are also among those most likely to be tested regularly. But HIV testing at a blood donation site could provide access and a safe friendly environment for non-gay people who might be a bit intimidated or uncomfortable asking their doctor or going to the testing center in the gay part of town.
February 17th, 2010
Anal cancer, a very rare condition, impacts gay men to a greater extent than heterosexuals (about 0.35% of gay men get anal cancer). The most significant contributor is infection with the Human Papillomavirus (HPV), the same virus that contributes to cervical cancer in women, causes genital warts, and is linked to some rare oral cancers in straight men. HPV is very common and most sexually active adults will be infected at some point in their life.
In October, the FDA approved the use of Gardasil, a vaccine, for males ages 9 through 26 for the prevention of genital warts. Now Merck has release testing results showing that the vaccine is significantly effective in the prevention of anal cancer in gay men.
Merck & Co., Inc. announced today that in new Phase III data, GARDASIL® [Human Papillomavirus Quadrivalent (Types 6, 11, 16 and 18) Vaccine, Recombinant] was 77.5 percent (95 percent CI: 39.6, 93.3) efficacious against anal intraepithelial neoplasia (AIN) associated with human papillomavirus (HPV) types 6, 11, 16 and 18 in 16-to-26 year-old men who have sex with men.
…
In this PPE analysis, GARDASIL prevented 77.5 percent (95 percent CI: 39.6, 93.3) of HPV 6, 11, 16, and 18-related AIN and anal cancer. A total of 29 men were diagnosed with HPV 6, 11, 16 or 18-related AIN during the study, with 24 cases in the placebo group and five in the vaccine group. No cases of HPV 11 or 18-related AIN were observed in the vaccine group. No cases of anal cancer were seen in either the placebo or vaccine group.
Most sexually active adults have been or will be infected with HPV. In most cases, the infection goes away naturally. But Merck also found that the vaccine efficacious in preventing infection in women aged 27 to 45, a demographic that is not yet approved by the FDA. It is easy to surmise that the next step will be to test men in this age group with the eventual goal of marketing to everyone.
Although the odds are low of getting HPV related cancer, it is probably to the advantage of all women and gay men to reduce those odds even further by getting vaccinated, if possible. While this may not be covered by your insurance, the $360 for the three shots may save your life.
This commentary is a personal rant from the author and may not necessarily reflect the opinion of other authors at Box Turtle Bulletin. Additionally, it is not directly within the realm of what this site normally covers. I wrote it anyway. I make no claim that this is representative of anyone else's story, but it's mine.
February 2nd, 2010
 In 2004 Aetna Insurance Company adopted the slogan, “We want you to know.” However, I really, really, truly, very much wish I knew nothing about Aetna.
In 2004 Aetna Insurance Company adopted the slogan, “We want you to know.” However, I really, really, truly, very much wish I knew nothing about Aetna.
As I wrote last Friday, Aetna, my HMO insurer, decided as of January 1, 2010 to move a medication that I require off of their preferred list. They do allow one other alternate medication, but I have an allergic reaction to that medication which results in redness and eye irritation and my ophthalmologist will not prescribe it.
In my update last Friday, I told you that it looked like a tier override might be possible. It is now clear that this was a misunderstanding. As I do not reside in New Jersey, such an option is not available.
During this process I discovered something interesting. Aetna has in place procedures to ensure that those who decide the pricing are shielded from all contact with those who suffer the consequences of their decisions. Even the intermediaries who speak with doctors are not allowed to talk to these decision makers, instead having all interaction be by means of forms and email.
Aetna wishes to make certain that those who deny coverage are not swayed by emotional appeal or the circumstances of any individual members. Were they to be made aware of the difficulties that they cause, they might be inclined to prioritize ethical practice ahead of gasp-worthy profits ($1.4 billion in 2008) and exorbitant executive salaries (which increased 625% between 2005 and 2008).
So Aetna wins. By taking my drug off the preference list, they will shift $25 per month from their bottom line to mine. And I have no recourse at all other than, of course, informing you, my Congressman, my Senators, my state legislators and the CA Insurance Commissioner of the practices of this corporation.
This commentary is a personal rant from the author and may not necessarily reflect the opinion of other authors at Box Turtle Bulletin. Additionally, it is not directly within the realm of what this site normally covers. I wrote it anyway. I make no claim that this is representative of anyone else's story, but it's mine.
January 29th, 2010
Most Americans have health insurance. And most Americans are content with their level of coverage. But “most” is not enough to quell the dissatisfaction that is growing in the nation over the way in which health issues are treated.
But unlike the politicians, I think the underlying discontent lies not in whether there is a single payer or whether catastrophic care is planned for or even in the increased cost of heath care. Rather, I think that the anger and frustration results from a total lack of control over ones own care coupled with the arrogance and condescension with which insurance companies treat the people who pay for their astronomic executive salaries and bonuses.
Allow me to illustrate.
I have pigmentary glaucoma. This is a rare genetic eye condition (discovered mostly in near-sighted male Caucasians in their 30s and 40s) in which bits of pigment flake off the iris and clog the eye’s drains. If untreated, the pressure in the eye builds, destroying the optic nerve and leading to blindness.
This is an easily treated disease. As long as I maintain a regimen of eye drops, I can keep the intraocular pressure in my eyes under control (below 21 mmHg) and avoid nerve damage. And although my eyes had reached pressures of 40 and 38 before detection, I have been very fortunate in that I have had very little loss of vision.
There are three different primary medications from which I can choose and, in the process of stabilizing my pressures, my doctor tried all of them. One was inadequately effective and one resulted in significant redness and irritation. But the third was, as Goldilocks might say, just right. (In conjunction with another eyedrop which works slightly differently)
So everything is just fine.
Until this week.
When I went to pick up my prescription I found that Aetna, my insurance provider, decided to move Travitan Z, one of my essential eye medications, off of their formulary list. What this means is that it is no longer covered at my standard deductible rate. In this case, the out-of-pocket monthly price of this medication went from $35 to $60.
Now moving a medication off the formulary list is not necessarily unreasonable. Sometime a generic is available, at other times there are comparable less expensive options that work identically. Unfortunately, this is not the case for me. There is no generic available and the alternatives were determined by my physician to be either less effective or a source of irritation.
So I called Aetna to discuss the situation. What I found was incompetence, arrogance, and condescension.
My first call resulted in a fellow telling me that he “went on Google” and found a generic, which would certainly have been fine with me. But after calling my pharmacy, I learned he had simply discovered the medication’s non-brand name but that this medication was not available as a generic drug and won’t be until 2013
The second call was when Aetna’s policy of deflecting criticism was revealed.
I was first told that the problem was due to my choices in the open enrollment period. So we walked through the options available that I so very foolishly ignored and, no surprise to me, in each option my eye coverage would be the same. Because the issue was not my “choices” at all, but rather that the drug had been moved off of the formulary list that was used for each of my options.
Having exhausted that avenue of blame, Aetna then told me, “that is the price at which your employer has chosen to cover that medication”. That, of course, was a flat out lie. My employer never said, “hmm, Travatan Z, yeah let’s raise the price on that”. Instead, my employer (or rather the large employment data processor that my real employer uses to process payroll benefits) set a rate for all non-formulary drugs and left the decision up to Aetna as to which drugs would be on the list.
The young lady to whom I was speaking then went for the “I didn’t decide that” route. Well, no, of course not.
But I wasn’t calling her to discuss my options, I was calling Aetna and she was just the voice of the company at that moment. But that simply generated another round of “well this is the result of your choices that you made during open enrollment and this is the amount your employer decided to pay for this drug”. It seems they trained her well; at no point did she acknowledge that the decision resulting in my increased co-pay was made by Aetna.
After finally having the young lady tell me that I had no options whatsoever, I thought for a moment about what I had hoped to achieve from my call. What could Aetna have done differently to avoid having me publicly vent my complaint?
In summation, I’m screwed. Aetna made a decision and I get to pay for that choice. I can pay more with a smile, or I can pay more and vent my frustration to the entire world (clearly, I’m choosing the latter).
Now I know that I am fortunate. Even after the increase, I’ll likely pay less than $2,000 out of pocket for medical care this year. Some people face monthly prescription costs in excess of that amount. It hardly seems worthy of this rant.
But my experience with Aetna addresses a bigger issue.
I am, by nature, favorable to capitalism. I believe that a system that rewards investment and research is more likely than any other to result in continued improvements in treatment for my condition. But capitalism relies on competition, on the ability of the customer to pick up their custom and go to the store next door, which is not an option that many Americans have.
And I do not object to insurance companies making a profit. It is reasonable that providing a service should be compensated. But egregious salaries and bonuses secured through a political system that secures insurers’ advantages and disallows or discourages cross-state shopping or foreign nation pricing are offensive if not downright immoral.
So I have now joined the ranks of those who think of health insurance companies, Aetna in particular, with contempt. Not because of what they provide or really even the profit they make, but because of the limitations on choices that lobbying has created and the arrogance and contempt that it has bred within a smug corporate culture confident that it need not compete for my patronage.
And unless insurers want moderates and conservatives to join with more collective-minded Americans and seek to dismantle the entire system, they should seriously rethink their approach to business.
UPDATE:
For those interested in the outcome, there may be a solution.
After ranting, I started searching the internet and Aetna’s own website and found that they had issued a Pharmacy Clinical Policy Bulletin which allowed for a medical exception specifically for glaucoma medicine if the patient was allergic to the one drug on their “preference list”. After reading this bulletin to Aetna’s employees, I was able to finally reach someone who was familiar with the exceptions that their customer service claimed did not exist.
After four calls from me (speaking to six different people) and two calls from my doctor, Aetna may be making a “tier override”. I’ve paid the larger co-pay but it looks like I may be refunded the difference.
But how many Aetna members do not have BTB readers to encourage them not to give up, are unskilled at searching, and are willing to believe what they are told by customer service? How many are just too sick to spend hours trying to resolve the problem?
Aetna should start caring about the concerns of their members. All the insurance companies should. In the current political culture, arrogance will not serve them well.
This commentary is the opinion of the author and does not necessarily reflect that of other authors at Box Turtle Bulletin.
November 9th, 2009
On Saturday, the US House of Representatives voted for the Affordable Health Care for America Act, a healthcare reform bill which has been the highest priority of the Democratic Party leadership since the party took control of the presidency and both houses of the legislature. There are a number of very positive inclusions in that bill, including some that deal specifically with the GLBT community.
Probably the most specifically significant to our community is the incorporation of the McDermott/Ros-Lehtinen bill to remove the special ‘gay couples tax\’ on spousal benefits provided by an employer. Currently, heterosexual spousal benefits are provided tax free and employers may claim them as an operating expense, but same-sex spousal benefits are considered to be part of the employee’s taxable income. This can result in thousands of dollars of tax demanded from our government solely because the spouse of the taxpayer is the same sex. Removing this tax is a tremendous relief on gay taxpayers.
Also included are changes in treatment for HIV patients, heath data collection related to the LGBT community, new sex education rules, and non-discrimination language.
However, the bill, as passed by the House, also provides for a “public option”, or insurance provision by the federal government. This government run health care mechanism is by far the most controversial aspect of the bill. And, depending on where you fall on the right/left scale, you may well have strong arguments either for or against such a move.
But while I have opinions in general about the decision on the part of the government to compete in the world of service provision, that is not the point of this commentary. Rather, I wish to express specific concerns about how this effort may impact our community negatively.
Featured Reports
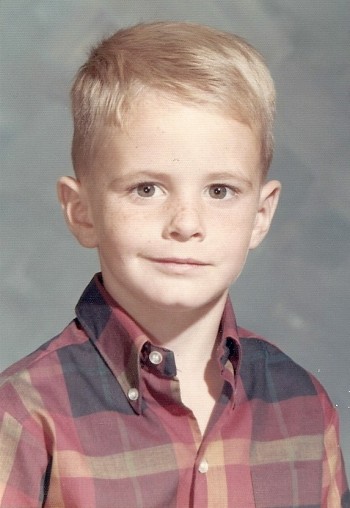 In this original BTB Investigation, we unveil the tragic story of Kirk Murphy, a four-year-old boy who was treated for “cross-gender disturbance” in 1970 by a young grad student by the name of George Rekers. This story is a stark reminder that there are severe and damaging consequences when therapists try to ensure that boys will be boys.
In this original BTB Investigation, we unveil the tragic story of Kirk Murphy, a four-year-old boy who was treated for “cross-gender disturbance” in 1970 by a young grad student by the name of George Rekers. This story is a stark reminder that there are severe and damaging consequences when therapists try to ensure that boys will be boys.
When we first reported on three American anti-gay activists traveling to Kampala for a three-day conference, we had no idea that it would be the first report of a long string of events leading to a proposal to institute the death penalty for LGBT people. But that is exactly what happened. In this report, we review our collection of more than 500 posts to tell the story of one nation’s embrace of hatred toward gay people. This report will be updated continuously as events continue to unfold. Check here for the latest updates.
In 2005, the Southern Poverty Law Center wrote that “[Paul] Cameron’s ‘science’ echoes Nazi Germany.” What the SPLC didn”t know was Cameron doesn’t just “echo” Nazi Germany. He quoted extensively from one of the Final Solution’s architects. This puts his fascination with quarantines, mandatory tattoos, and extermination being a “plausible idea” in a whole new and deeply disturbing light.
On February 10, I attended an all-day “Love Won Out” ex-gay conference in Phoenix, put on by Focus on the Family and Exodus International. In this series of reports, I talk about what I learned there: the people who go to these conferences, the things that they hear, and what this all means for them, their families and for the rest of us.
Prologue: Why I Went To “Love Won Out”
Part 1: What’s Love Got To Do With It?
Part 2: Parents Struggle With “No Exceptions”
Part 3: A Whole New Dialect
Part 4: It Depends On How The Meaning of the Word "Change" Changes
Part 5: A Candid Explanation For "Change"
 At last, the truth can now be told.
At last, the truth can now be told.
Using the same research methods employed by most anti-gay political pressure groups, we examine the statistics and the case studies that dispel many of the myths about heterosexuality. Download your copy today!
And don‘t miss our companion report, How To Write An Anti-Gay Tract In Fifteen Easy Steps.
 Anti-gay activists often charge that gay men and women pose a threat to children. In this report, we explore the supposed connection between homosexuality and child sexual abuse, the conclusions reached by the most knowledgeable professionals in the field, and how anti-gay activists continue to ignore their findings. This has tremendous consequences, not just for gay men and women, but more importantly for the safety of all our children.
Anti-gay activists often charge that gay men and women pose a threat to children. In this report, we explore the supposed connection between homosexuality and child sexual abuse, the conclusions reached by the most knowledgeable professionals in the field, and how anti-gay activists continue to ignore their findings. This has tremendous consequences, not just for gay men and women, but more importantly for the safety of all our children.
Anti-gay activists often cite the “Dutch Study” to claim that gay unions last only about 1½ years and that the these men have an average of eight additional partners per year outside of their steady relationship. In this report, we will take you step by step into the study to see whether the claims are true.
Tony Perkins’ Family Research Council submitted an Amicus Brief to the Maryland Court of Appeals as that court prepared to consider the issue of gay marriage. We examine just one small section of that brief to reveal the junk science and fraudulent claims of the Family “Research” Council.
 The FBI’s annual Hate Crime Statistics aren’t as complete as they ought to be, and their report for 2004 was no exception. In fact, their most recent report has quite a few glaring holes. Holes big enough for Daniel Fetty to fall through.
The FBI’s annual Hate Crime Statistics aren’t as complete as they ought to be, and their report for 2004 was no exception. In fact, their most recent report has quite a few glaring holes. Holes big enough for Daniel Fetty to fall through.