Box Turtle Bulletin
 News and commentary about the anti-gay lobby
News and commentary about the anti-gay lobby News and commentary about the anti-gay lobby
News and commentary about the anti-gay lobbyThis commentary is a personal rant from the author and may not necessarily reflect the opinion of other authors at Box Turtle Bulletin. Additionally, it is not directly within the realm of what this site normally covers. I wrote it anyway. I make no claim that this is representative of anyone else's story, but it's mine.
January 29th, 2010
Most Americans have health insurance. And most Americans are content with their level of coverage. But “most” is not enough to quell the dissatisfaction that is growing in the nation over the way in which health issues are treated.
But unlike the politicians, I think the underlying discontent lies not in whether there is a single payer or whether catastrophic care is planned for or even in the increased cost of heath care. Rather, I think that the anger and frustration results from a total lack of control over ones own care coupled with the arrogance and condescension with which insurance companies treat the people who pay for their astronomic executive salaries and bonuses.
Allow me to illustrate.
I have pigmentary glaucoma. This is a rare genetic eye condition (discovered mostly in near-sighted male Caucasians in their 30s and 40s) in which bits of pigment flake off the iris and clog the eye’s drains. If untreated, the pressure in the eye builds, destroying the optic nerve and leading to blindness.
This is an easily treated disease. As long as I maintain a regimen of eye drops, I can keep the intraocular pressure in my eyes under control (below 21 mmHg) and avoid nerve damage. And although my eyes had reached pressures of 40 and 38 before detection, I have been very fortunate in that I have had very little loss of vision.
There are three different primary medications from which I can choose and, in the process of stabilizing my pressures, my doctor tried all of them. One was inadequately effective and one resulted in significant redness and irritation. But the third was, as Goldilocks might say, just right. (In conjunction with another eyedrop which works slightly differently)
So everything is just fine.
Until this week.
When I went to pick up my prescription I found that Aetna, my insurance provider, decided to move Travitan Z, one of my essential eye medications, off of their formulary list. What this means is that it is no longer covered at my standard deductible rate. In this case, the out-of-pocket monthly price of this medication went from $35 to $60.
Now moving a medication off the formulary list is not necessarily unreasonable. Sometime a generic is available, at other times there are comparable less expensive options that work identically. Unfortunately, this is not the case for me. There is no generic available and the alternatives were determined by my physician to be either less effective or a source of irritation.
So I called Aetna to discuss the situation. What I found was incompetence, arrogance, and condescension.
My first call resulted in a fellow telling me that he “went on Google” and found a generic, which would certainly have been fine with me. But after calling my pharmacy, I learned he had simply discovered the medication’s non-brand name but that this medication was not available as a generic drug and won’t be until 2013
The second call was when Aetna’s policy of deflecting criticism was revealed.
I was first told that the problem was due to my choices in the open enrollment period. So we walked through the options available that I so very foolishly ignored and, no surprise to me, in each option my eye coverage would be the same. Because the issue was not my “choices” at all, but rather that the drug had been moved off of the formulary list that was used for each of my options.
Having exhausted that avenue of blame, Aetna then told me, “that is the price at which your employer has chosen to cover that medication”. That, of course, was a flat out lie. My employer never said, “hmm, Travatan Z, yeah let’s raise the price on that”. Instead, my employer (or rather the large employment data processor that my real employer uses to process payroll benefits) set a rate for all non-formulary drugs and left the decision up to Aetna as to which drugs would be on the list.
The young lady to whom I was speaking then went for the “I didn’t decide that” route. Well, no, of course not.
But I wasn’t calling her to discuss my options, I was calling Aetna and she was just the voice of the company at that moment. But that simply generated another round of “well this is the result of your choices that you made during open enrollment and this is the amount your employer decided to pay for this drug”. It seems they trained her well; at no point did she acknowledge that the decision resulting in my increased co-pay was made by Aetna.
After finally having the young lady tell me that I had no options whatsoever, I thought for a moment about what I had hoped to achieve from my call. What could Aetna have done differently to avoid having me publicly vent my complaint?
In summation, I’m screwed. Aetna made a decision and I get to pay for that choice. I can pay more with a smile, or I can pay more and vent my frustration to the entire world (clearly, I’m choosing the latter).
Now I know that I am fortunate. Even after the increase, I’ll likely pay less than $2,000 out of pocket for medical care this year. Some people face monthly prescription costs in excess of that amount. It hardly seems worthy of this rant.
But my experience with Aetna addresses a bigger issue.
I am, by nature, favorable to capitalism. I believe that a system that rewards investment and research is more likely than any other to result in continued improvements in treatment for my condition. But capitalism relies on competition, on the ability of the customer to pick up their custom and go to the store next door, which is not an option that many Americans have.
And I do not object to insurance companies making a profit. It is reasonable that providing a service should be compensated. But egregious salaries and bonuses secured through a political system that secures insurers’ advantages and disallows or discourages cross-state shopping or foreign nation pricing are offensive if not downright immoral.
So I have now joined the ranks of those who think of health insurance companies, Aetna in particular, with contempt. Not because of what they provide or really even the profit they make, but because of the limitations on choices that lobbying has created and the arrogance and contempt that it has bred within a smug corporate culture confident that it need not compete for my patronage.
And unless insurers want moderates and conservatives to join with more collective-minded Americans and seek to dismantle the entire system, they should seriously rethink their approach to business.
UPDATE:
For those interested in the outcome, there may be a solution.
After ranting, I started searching the internet and Aetna’s own website and found that they had issued a Pharmacy Clinical Policy Bulletin which allowed for a medical exception specifically for glaucoma medicine if the patient was allergic to the one drug on their “preference list”. After reading this bulletin to Aetna’s employees, I was able to finally reach someone who was familiar with the exceptions that their customer service claimed did not exist.
After four calls from me (speaking to six different people) and two calls from my doctor, Aetna may be making a “tier override”. I’ve paid the larger co-pay but it looks like I may be refunded the difference.
But how many Aetna members do not have BTB readers to encourage them not to give up, are unskilled at searching, and are willing to believe what they are told by customer service? How many are just too sick to spend hours trying to resolve the problem?
Aetna should start caring about the concerns of their members. All the insurance companies should. In the current political culture, arrogance will not serve them well.
Latest Posts
Featured Reports
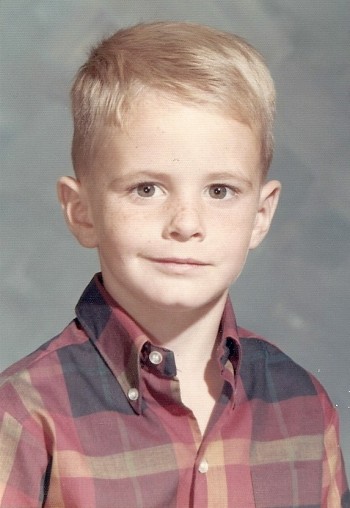 In this original BTB Investigation, we unveil the tragic story of Kirk Murphy, a four-year-old boy who was treated for “cross-gender disturbance” in 1970 by a young grad student by the name of George Rekers. This story is a stark reminder that there are severe and damaging consequences when therapists try to ensure that boys will be boys.
In this original BTB Investigation, we unveil the tragic story of Kirk Murphy, a four-year-old boy who was treated for “cross-gender disturbance” in 1970 by a young grad student by the name of George Rekers. This story is a stark reminder that there are severe and damaging consequences when therapists try to ensure that boys will be boys.
When we first reported on three American anti-gay activists traveling to Kampala for a three-day conference, we had no idea that it would be the first report of a long string of events leading to a proposal to institute the death penalty for LGBT people. But that is exactly what happened. In this report, we review our collection of more than 500 posts to tell the story of one nation’s embrace of hatred toward gay people. This report will be updated continuously as events continue to unfold. Check here for the latest updates.
In 2005, the Southern Poverty Law Center wrote that “[Paul] Cameron’s ‘science’ echoes Nazi Germany.” What the SPLC didn”t know was Cameron doesn’t just “echo” Nazi Germany. He quoted extensively from one of the Final Solution’s architects. This puts his fascination with quarantines, mandatory tattoos, and extermination being a “plausible idea” in a whole new and deeply disturbing light.
On February 10, I attended an all-day “Love Won Out” ex-gay conference in Phoenix, put on by Focus on the Family and Exodus International. In this series of reports, I talk about what I learned there: the people who go to these conferences, the things that they hear, and what this all means for them, their families and for the rest of us.
Prologue: Why I Went To “Love Won Out”
Part 1: What’s Love Got To Do With It?
Part 2: Parents Struggle With “No Exceptions”
Part 3: A Whole New Dialect
Part 4: It Depends On How The Meaning of the Word "Change" Changes
Part 5: A Candid Explanation For "Change"
 At last, the truth can now be told.
At last, the truth can now be told.
Using the same research methods employed by most anti-gay political pressure groups, we examine the statistics and the case studies that dispel many of the myths about heterosexuality. Download your copy today!
And don‘t miss our companion report, How To Write An Anti-Gay Tract In Fifteen Easy Steps.
 Anti-gay activists often charge that gay men and women pose a threat to children. In this report, we explore the supposed connection between homosexuality and child sexual abuse, the conclusions reached by the most knowledgeable professionals in the field, and how anti-gay activists continue to ignore their findings. This has tremendous consequences, not just for gay men and women, but more importantly for the safety of all our children.
Anti-gay activists often charge that gay men and women pose a threat to children. In this report, we explore the supposed connection between homosexuality and child sexual abuse, the conclusions reached by the most knowledgeable professionals in the field, and how anti-gay activists continue to ignore their findings. This has tremendous consequences, not just for gay men and women, but more importantly for the safety of all our children.
Anti-gay activists often cite the “Dutch Study” to claim that gay unions last only about 1½ years and that the these men have an average of eight additional partners per year outside of their steady relationship. In this report, we will take you step by step into the study to see whether the claims are true.
Tony Perkins’ Family Research Council submitted an Amicus Brief to the Maryland Court of Appeals as that court prepared to consider the issue of gay marriage. We examine just one small section of that brief to reveal the junk science and fraudulent claims of the Family “Research” Council.
 The FBI’s annual Hate Crime Statistics aren’t as complete as they ought to be, and their report for 2004 was no exception. In fact, their most recent report has quite a few glaring holes. Holes big enough for Daniel Fetty to fall through.
The FBI’s annual Hate Crime Statistics aren’t as complete as they ought to be, and their report for 2004 was no exception. In fact, their most recent report has quite a few glaring holes. Holes big enough for Daniel Fetty to fall through.
CPT_Doom
January 29th, 2010
I work in the health care industry with a lot of contact with insurers (and no, we don’t get better coverage just because we’re “in the know”). You need to realize you are not their client – your employer is. It is the employer that decides what insurer(s) to offer (some organizations offer choices, most don’t) and it is the employer who has to pay the lion’s share of the premium. Taking expensive drugs off formulary is one way to reduce premiums and shift costs to consumers, which reduces costs to the employer.
However, you do have two options. Aetna HAS to provide an exceptions process for their formulary decisions. Because your doctor has already tried the other available medications and they have not worked, you would normally be eligible for such an exception (which should reduce your out-of-pocket expenses). You should definitely enlist your physician’s office in this endeavor, they have likely dealt with this before. Assuming Aetna has a web site, they should explain the exceptions process on it.
The other route is to go through your HR department. You are right that the employer does not know all the changes that lead to their premiums, but you can enlist the employer to intervene with the insurer – after all, the employer is the customer. I would lay this all out with whoever in HR is responsible for benefit decisions.
Timothy Kincaid
January 29th, 2010
Thanks, CPT_Doom
The lovely young lady with whom I spoke told me “no exceptions”. Let’s hope she was ill informed and that this wasn’t just what she was trained to say.
B John
January 29th, 2010
Timothy…do not for one minute accept as accurate what you hear from customer service people. My experience is they are rarely accurate. Despite what insurers will claim, those folks are in a sweat-shop call center and are NOT measured based on customer satisfaction. That would be too hard. They are measured based on a report the computer generates telling the supervisor how many calls per hour were handled by that operator. It’s easy and objective. The CSR’s know the game, and they work the pay plan.
So there job is not to help you, but get you off the phone having given you some explanation that hopefully keeps you from calling back.
Never accept the first or second or answer you receive…escalate. Demand to hear from the companies Medical Director.
Priya Lynn
January 29th, 2010
As a Canadian I look at the U.S. health care situation with stunned amazement – so many Americans want to shoot themselves in the foot by opposing universal health care. They falsely claim health care is rationalized in countries like Canada when the opposite is true. I’ve never been denied any health care service, drug, or precedure I’ve needed and it is Americans who I constantly hear about being denied serivce for ‘pre-existting conditions’ and whatever other excuse the insurance company can come up with to deny people what they need. The Americans I know live in fear of needing treatment and not being able to afford it, I haven’t the slightest fear of that in my country.
Karen
January 29th, 2010
Do not assume that the person you spoke with is uninformed if you are given incorrect information. Keep pushing. Insurance companies can avoid paying if they can convince people the case is hopeless.
Priya Lynn
January 29th, 2010
If I recall correctly roughly 60 million Americans don’t have health insurance so its rather misleading for Timoty to start this post with “Most Americans have health insurance. And most Americans are content with their level of coverage.” – that’s an unconscienable number of Americans in a tenuous situation. Americans like to brag about how their’s is the greatest country in the world, not with realities like that it isn’t.
Burr
January 29th, 2010
This is exactly the problem with the insurance system here. We have no choices and are held hostage to employment-based insurance and state coverage mandates.
Anyone claiming this is a free market and the problems are a result of it is a fool. And ObamaCare would have done nothing but force everyone to buy a product that doesn’t work for them.
I would prefer a single payer system compared to what we have now, but I also would prefer a true free market. Give me my full salary and let me shop. If you want to bring costs down, you need to stop hiding them from the consumer.
pantherq
January 29th, 2010
Insurance companies should not decide treatment. Period.
Neko
January 29th, 2010
At least you have insurance? I’m a 25 year old full-time student who is too old to be on my parents’ insurance plans, and who goes to a school that doesn’t offer insurance. So… I’m kind of screwed. I’ve been rejected from all the individual plans I have applied for because I have pre-existing conditions. Which are, uh… as far as we can tell? Migraines and an anxiety disorder. With a side of having constant ear infections when I was a kid.
Not having insurance is terrifying. I know that if I get hurt or sick, there’s not really anything I can do. I can’t afford to go to the hospital ($5000 just to walk in the door), and I can’t afford a doctor ($80 for a basic office visit… around $500 if they need to do bloodwork). I actually had a UTI about a month ago that got really bad because I couldn’t do anything about it… until my mother got me antibiotics by lying to her doctor about needing a refill of her own. Considering my mother is a lot larger than be, it’s entirely possible that I was being given an overdose, but… whatever.
It’s not just the individual companies that are messed up. The entire system really does need an overhaul. Insurance companies like to reject people, drop people, drop medications, and basically do everything possible to not shell out money. It’s horrible.
AJD
January 29th, 2010
Priya,
I’ve always thought “America is the greatest nation in the world” was such an empty, stupid catchphrase. I mean, a lot of countries have civil liberties comparable to ours, lots of natural beauty and a high standard of living…and on top of that, a lot of them also have universal health care, high-speed trains (by which I mean actual bullet trains traveling at 125mph or faster, not the pathetic excuse for “high-speed rail” that got $8 billion in the stimulus bill), better public education, better infrastructure overall, richer cultures, better food, gay marriage and so on.
That’s not to say I’m anti-American or miserable living here, but that catchphrase has always gone alongside “Love it or leave it” as the sort of thing people say when they don’t know a whole lot about the rest of the world and/or are satisfied with poor quality because it’s what they’re used to and thus see no need for improvement.
Gary Brewton MD FACP
January 29th, 2010
Paraphrasing Daniel and recontextualizing:
“The fingers of a human hand appeared and began writing on the walls of the board rooms of the health insurance companies. And this is the writing that was inscribed: mene, mene, tekel, and parsin. And the interpreter told the bosses of the insurance companies: You have exalted yourself over the vulnerable ones you promised to protect, and you have made your hearts stone. Because you love money more than justice, this is the judgment: mene, God has numbered the days of your business empire and brought it to an end; tekel, you have been weighed on the scales and found wanting; peres, your business empire is divided and taken from you.”
Emily K
January 29th, 2010
I pay for 3 Rx’s to keep me from killing myself or others. I suffer from a severe mental illness that has on many occasions, almost overcome me. Each time I’m able to overcome it. (so far.) My medications are NOT cheap; one is not close to being a generic according to patent law. My parents pay for my health insurance, which I do not have because 1) for years I freelanced and got by by the skin of my teeth, skating just above poverty, and 2) until last week I was not an “official” permanent employee at my current (new) job.
Every day I consider moving to another country so that I can afford to pay for my drugs, and work at a job where the minimum wage is higher than $7-something.
Maybe someday I’ll make that happen.
Tim, I’m very sorry you are going through this.
grantdale
January 29th, 2010
Well yess… but only half-flippantly that’s because United States health insurance companies aren’t actually in the ‘insurance’ business.
Jeepers, we (the ENTIRE rest of the developed World) realised this decades ago and introduced the proven solution. It’s effective. It’s efficient. And it works for everyone except… the private health insurance companies, and maybe people earning $28 million per year.
(Note to self: one of the biggest avoidable burdens on your system are the transaction costs. A screwed-up and inefficient system takes a lot of $ to simply churn around the paper and answer the phones to pissed-off ‘customers’. I’m not even going to start on about the personal costs to an individual if they happen to come down with a condition and then lose their job or have to change insurers. Or if their insurer simply decides to cut off a benefit, like they just did to you.)
Timothy — if you’re up for the challenge… I’d be more than happy to compare the two total system costs (including taxes): yours, wholly privately insured + out-of-pocket and ours, a mix of Medicare + top-up private insurance (our choice) + out-of-pocket. Us versus you. Direct comparison.
Hey, you’re a numbers man… we know you love this type of stuff!
No need to spread it all over the internet, you’ve got our email :)
———————
(simply out of curiosity: all figures in US dollars)
Travatan: a PBS drug, so you’d pay $30 a pop ($4.80 if you were my mother), with the PBS topping that up by $38. The drug co gets $68.
You’d also pay a max of $1150 out-of-pocket expenses for any and all prescriptions per year as a single person. Or the same as a family unit — couples (same or opp), including any kids. Anything over that $1150 per year per family unit is covered.
(This max drops to $290 per year for pensioners, health care card holders etc. Again covering the whole family unit.)
As a US citizen you’d pay the whole $68 when visiting but citizens of Italy, New Zealand, Ireland, Finland, Malta, the Netherlands, Sweden, Norway, the United Kingdom and Belgium enjoy reciprocal arrangements for prescriptions and pay the same as we do.
Richard W. Fitch
January 29th, 2010
grantdale, where are you? Any good real estate values in the neighborhood?
grantdale
January 29th, 2010
/ha. Yes, that may have been helpful: Australia. And for Q2, probably. Or not. Are you buying or selling? :)
cd
January 29th, 2010
If I recall correctly roughly 60 million Americans don’t have health insurance so its rather misleading for Timothy to start this post with “Most Americans have health insurance. And most Americans are content with their level of coverage.â€
It is technically correct, though it would be morally correct to add “And the Americans satisfied with things as they are those who choose to be blind to the grotesque cost-shifting, contract breaching, free riding, abusive billing, and inefficiency for all that now defines the system.”
Trevor
January 30th, 2010
As we know we’re better off under the current system. Why if the guverment provided health insurance we’d all have to stand before the “Death Panel”. Private insurance companies “never” deny the best and latest treatment afterall. What possible motive could they have for denying expensive albeit life-saving treatment? And even if they did, isn’t that a better way than single-payer? Socialism won’t keep the CEO on gold-plated yachts you know.
lurker
January 30th, 2010
I had a similar problem . . . a very standard drug I use for a chronic condition was taken off the BS/BS formulary. No generic. Nothing else remotely in the same drug class. This is a low potency/low risk drug that worked for me. My out of pocket cost for a 1-month supply now? $300.00.
When I called to complain the rep told me that it was off the formulary now because the drug did not meet the BS/BS “pharmico economic” value. F**ing BS for “it’s too expensive and we don’t want to pay for it.”
I’m not with BS/BS any more.
lurker
January 30th, 2010
* BS/BS: Blue s**t/Blue shield
lurker
January 30th, 2010
does make you wonder about that gov’t mandate to make everyone buy health insurance. Yes, we’ll all have to pay IN, but what will the insurers have to pay OUT? Maybe not much. Devil’s in those details.
Ben Mathis
January 30th, 2010
Not only have other people covered the fact that in one of the nations with the most wealth in the world (in the hands of 1% of it’s population) has 60 million without coverage, 42,000 dying ever year for lack of basic care, 60% of all bankrupties from healthcare costs of which 75% of them had some type of healthcare insurance coverage, BUT you are wrong about capitalism providing the R&D for new drugs. 70% of funding for new drugs comes from government grants, and as such is socialized in it’s development. Drug companies spend very little of their returns on R&D, instead spending it on advertisement and ways to flout the system with new drugs that are slight tweaks on old ones.
The American healthcare provision systems is completely failed in every way and some 3rd would countries enjoy better care. Certainly ever 1st world country enjoys healthcare a multitude better in quality and quantity, so any arguments for America’s model is not only flawed but disgusting.
Jason D
January 30th, 2010
I don’t have health insurance.
But when I did, I barely used it.
I work out, I don’t have any potentially dangerous hobbies like rock climbing. I go to bed early, I eat (not great but) pretty good food often, I don’t drink, and I quit smoking. I’ve never had an STD, I don’t even have that mildly irritating form of herpes that the majority of the population presumably has.
I’ve seen so much arrogant commenting (not here) from people who are in a similar situation to mine.
They would say that those expensive medical bills are because ya’ll are living unhealthy lifestyles! If you just drink water and jump on the treadmill 3 times a week, everything would be hunky dory!
They forget that health conditions are not a sign of unhealthy living. Why do people still have this medieval belief that if something goes wrong in your life, it’s because you deserve it? Whether it’s a health problem, being less than attractive, or an earthquake, it’s like they think people deserve the challenges they face, rather than them simply being the given circumstances of someone’s life.
I think it’s this weird leftover from puritanism, that we get punished for stepping out of line, and rewarded for being perfect.
The healthcare debate has really brought out the racist, classist, and arrogant selfishness of a lot of people.
ZRAinSWVA
January 30th, 2010
My spouse is self employed and currently pays $563/month for health insurance. It increases roughly $70/month/year. And that’s before any co-pays he might incur during the course of the year–which are substantial because he chose higher co-pays to reduce the premium costs. Unfortunately, he cannot ‘shop around’ because of preexisting conditions which any new insurer would not cover.
It’s an incredibly frustrating situation.
Joe G.
January 30th, 2010
Timothy,
Although I’m glad to read that you have an option (as pointed out by CPT_Doom) nonetheless, people facing serious health problems should not have to go through this. It’s enough just managing the condition itself. We experience a lot of stress when we are faced with having to defend the need for something that can help us manage the medical condition.
Deplorable.
grantdale
January 30th, 2010
ZRAinSWVA
Just by rough comparison, the TWO of us — Medicare levy on both our incomes + proportion of taxes to cover the tax gap + our own choice to take out private insurance to remove/reduce co-pays … is roughly even with what your husband pays for himself. Plus he also pays a proportion of taxes to cover your own (distorted) ‘public’ schemes. And he still has co-pays.
(We have no deductions for children etc and get whacked the full amount in tax.)
And a 12%+ increase per year as well, for the privilege of being a captured customer???
Just to rub it in… for our money we not only get get comprehensive cover, and low and limited out-of-pocket costs, but we also get the bizarre pleasure of knowing that all our fellow citizens are covered by a good universal scheme.
Half the price per head for better total lifelong universal health cover…
Let me off at the next stop. I’ve heard enough.
You good people are being raped blind.
ZRAinSWVA
January 30th, 2010
Grantdale, agreed, and I’m ready to move!
And, no, I neglected to include the ‘self-employment tax (medicare and social security), which topped $7500 last year. (sigh)
Richard Rush
January 30th, 2010
Here is my little story. It is very minor compared to others, but I think it demonstrates the systematic intimidation, stonewalling, and exploitation of vulnerable people that has become the modus operandi for insurance companies. I must concede, however, that my story provides no actual proof of this.
After an accident in 2004 that required a titanium plate fastened with ten screws in my arm, I began a period of out-patient rehab three times a week. My Blue Cross plan covered 30 sessions per year with a $40 co-pay for each one.
After about twelve rehab visits I received a written notice from BC stating “The maximum benefit for this type of service has been reached.” I called BC and the person agreed that there was an error and that I was indeed entitled to thirty visits.
Two weeks later I received another notice. I called BC again, and the person again acknowledged the error.
Then after another three weeks – you guessed it. Similar conversation with BC, but this time the phone person made me feel really confident that the matter would be corrected. I felt relieved. But it was not to be.
Then there was a fourth notice and later a fifth notice. I just ignored them, and after that, they never bothered me about it again. And I did utilize 29 of my 30 visits.
I cannot believe that BC could be this incompetent, and thus I believe it is harassment that is actually designed to intimidate, stonewall, and exploit vulnerable people into not using the services to which they are entitled. And I don’t think the phone people are in on the scam – I think they genuinely tried to correct what they knew was an error.
As the anecdotal evidence against the insurance companies continues to mount, it is rapidly becoming a mountain of compelling evidence.
Ben Mathis
January 30th, 2010
I’m still boggled that someone could write, “Insurance company arrogance is one big reason people are unhappy about healthcare”. It’s possibly number 50 on the list of problems, if even that high. People having no coverage, insufficient coverage, being hassled non stop when in a time of sickness or poor health, not having coverage for a spouse or child or parent, longer wait times for General Practitioners, specialists, and surgery, all of these are real problems Americans face that I’m sure cause a great deal more unhappiness than just the arrogance the insurance companies show to their captive customers. I’m sure it’s irritating, but the people dying in the gutter for lack of healthcare are probably just a smidgen more irritated.
As an American moved to Europe, I’m so glad that even though I’m in good health now while I’m young, I never have to worry about healthcare costs for myself or my legally married husband for our entire lives.
CLS
January 30th, 2010
Bad as that is wait until you have to ask government bureaucrats for care. One person above gets it very right. You are not the client. When govt. regulated health care they pushed it into the employers hands, not your hands. So you don’t matter. Health care needs to return to the individual. It needs to be made tax deductible for each individual, not just for employers. And, it is time to end cartels in each state by legalizing competition across state lines. And, contrary to the amazement of Canadians, studies of treatment rates do show that Americans, with all the flaws of state regulation here, have HIGHER treatment rates for the diseases studied than do Canadians for the same illness.
Ben Mathis
January 30th, 2010
CLS, you need to check your facts. Canadians have longer life spans, lower infant mortality, shorter wait times to see doctors, specialists and surgeons.
Competing across state lines is what has ruined credit cards, because every state competes for the company’s business by killing taxes and regulations. This would in affect create yet another race to the bottom as all insurance companies move to the state with the least regulations and taxes.
The better question is why is anyone at all concerned with the businesses that got us in this mess? They make money by NOT providing care. It’s a ridiculous business model that should be kept away from essential services such as healthcare. These are blood sucking leeches that are funneling money into the top .1% at the expense of millions of Americans and should be dismantled and scattered in the wind.
Richard Rush
January 30th, 2010
CLS said, “Bad as that is wait until you have to ask government bureaucrats for care.”
I have been chauffeuring my elderly mother around for her medical care for years. She is 91 now and recently went into a nursing home.
With GOVERNMENT Medicare and supplemental Medigap insurance, there have been absolutely no problems at all. None. And the nursing home is a state GOVERNMENT owned/run facility with over 700 residents, and the care is excellent. It’s so good that many people choose to go there on a private-pay basis because the care is superior to many private nursing homes.
But there was one problem she had a number of years ago – it involved insurance companies. She had been on Medicaid in addition to Medicare, but when her financial situation improved and she no longer qualified for Medicaid, Blue Cross and others refused to sell her a Medigap policy. Only AARP/United HealthCare would sell her a policy.
I turned 65 last year which means I am now on GOVERNMENT Medicare. There are few things wonderful about getting old, but Medicare is one of them. I’m self-employed and I’m relieved to be finished with the private insurance quagmire. Of course, I do have private Medigap insurance to cover the 20% that Medicare does not, but that is an area that the private companies manage to do well (thanks to GOVERNMENT regulation).
I should note that my mother and I have traditional Medicare (as I believe most people do), not one of the Medicare “Advantage” plans that were created by Republicans during the Bush years. Anyone younger than 65 that likes their private HMO will absolutely love an “Advantage” plan when they turn 65. The “Advantage” plan option turns Medicare coverage over to private companies so you can enjoy all the advertising deception and subsequent intimidation, stonewalling, and exploitation of vulnerable people that you enjoyed with your HMO.
paul j stein
January 30th, 2010
After filing for hearings for 9 months,4 hearing,4 episodes of lost paperwork, the hearing officer was going to rule in my favor for a $410 pain med prescription i had paid for 9 months earlier. Her BOSS overruled her with the phrase “IF WE DO IT FOR HIM WE WILL HAVE TO DO IT FOR ALL OF HIS CLASS OF PATIENTS”. Ohio MEDICAID managed care system. Now starting next month they are going back to the previous system I was filing hearings to force them to get back onto. Too damn many steps(persons) between the patient and the meds and the costs were going higher and higher. Simple is better!
Doug
February 1st, 2010
Timothy, you write:
“I am, by nature, favorable to capitalism.”
I would question the assumption that having a favorable opinion on capitalism is an inborn trait (that is, “by nature”). I say this not to split hairs, but to suggest that maybe you prefer capitalism because it’s what you’re familiar with and have been taught to believe is best, supplemented by some observations made throughout your life.
I would also like to point out that Aetna is a corporation, and that its main obligation is to its shareholders. It was created to make money.
Lefty Kevin in UK
February 1st, 2010
Wow, sounds an awful and authoritarian system you have. I expect you have those “death panels” – you know, the committees that tell people they can’t get any more help so they have to die.
Surely a health system is intended to maintain the health of the whole community? Don’t you see how that protects everyone and is cheaper in the long run?
You can’t just intend the poor to die – can you?
What a country – call yourselves Christian? There’s a laugh!
Leave A Comment