Box Turtle Bulletin
 News and commentary about the anti-gay lobby
News and commentary about the anti-gay lobby News and commentary about the anti-gay lobby
News and commentary about the anti-gay lobbyThis commentary is the opinion of the author and does not necessarily reflect that of other authors at Box Turtle Bulletin.
March 8th, 2010
 In 1983, the FDA established a policy requiring that blood banks not accept donations from any male who had engaged in sex with any other man at any point since 1977. This was implemented so as to attempt to eliminate blood which was potentially infected with the HIV virus from the pool, and it made sense at that time.
In 1983, the FDA established a policy requiring that blood banks not accept donations from any male who had engaged in sex with any other man at any point since 1977. This was implemented so as to attempt to eliminate blood which was potentially infected with the HIV virus from the pool, and it made sense at that time.
It wasn’t until 1983 that the HIV virus was identified, and a method of testing for the virus wasn’t established for another two years.
In 2006, the AABB, America’s Blood Centers, and American Red Cross jointly asked the FDA to reconsider these rules. They argued that continuing the ban was not justified by scientific advances since the ban was implemented.
AABB, ABC and ARC believe that the current lifetime deferral for men who have had sex with other men is medically and scientifically unwarranted and recommend that deferral criteria be modified and made comparable with criteria for other groups at increased risk for sexual transmission of transfusion-transmitted infections. Presenting blood donors judged to be at risk of exposure via heterosexual routes are deferred for one year while men who have had sex with another man even once since 1977 are permanently deferred.
Current duplicate testing using NAT and serologic methods allow detection of HIV- infected donors between 10 and 21 days after exposure. Beyond this window period, there is no valid scientific reason to differentiate between individuals infected a few months or many years previously. The FDA-sanctioned Uniform Donor History Questionnaire was developed recognizing the importance of stimulating recall of recent events to maximize the identification of donors at risk for incident, that is, recent, infections. From the perspective of eliciting an appropriate risk history for exposure to HIV and other sexually transmitted infections, the critical period is the three weeks immediately preceding donation since false negative NAT and serology reflect these window-period infections, and the length of these window periods provide the scientific basis for the deferral periods imposed for at risk sexual behaviors.
The FDA refused.
They argue that as gay men have a higher concentration of HIV infection than some other demographics, this justifies a blanket ban on all donations by all gay men.
Men who have had sex with men since 1977 have an HIV prevalence (the total number of cases of a disease that are present in a population at a specific point in time) 60 times higher than the general population, 800 times higher than first time blood donors and 8000 times higher than repeat blood donors (American Red Cross). Even taking into account that 75% of HIV infected men who have sex with men already know they are HIV positive and would be unlikely to donate blood, the HIV prevalence in potential donors with history of male sex with males is 200 times higher than first time blood donors and 2000 times higher than repeat blood donors.
This week, Senator John Kerry, along with several other Senators, sent a letter to the FDA requesting that they reconsider their rules.
“Not a single piece of scientific evidence supports the ban,” the Democratic senator said in a statement. “A law that was once considered medically justified is today simply outdated and needs to end, just as last year we ended the travel ban against those with HIV.”
I doubt that this will be effective. If the FDA refuses to listen to those who know the very most about donation, testing, infection, and the blood supply, why would they listen to John Kerry?
But Kerry’s action does allow us as a nation to re-question why the ban is in place. Is it a matter of heath science or a matter of mistrusting (or disliking) gay men?
The FDA argues that any increased risk of tainting the supply is unacceptable. And that allowing gay men to contribute would unquestionably increase that risk.
But is that true? Does the ban effectively increase the safety of our blood supply? Or does it actually do harm?
To answer these questions, I think we need to look closer at the ban and how it functions.
1. The ban is only as effective as it is perceived to be reasonable. Remember, the ban is voluntary; by that, I mean that the only thing which stops donation is a questionnaire and the donor’s decision to answer honestly. If a gay man is determined to donate, he will only be persuaded not to donate if he believes that the criteria of exclusion is based on reason and not on bias.
2. We must assume that only a psychopath would choose to purposefully donate HIV infected blood. And no questionnaire is going to stop a psychopath. Therefore, this purpose of the questions is to eliminate those who are unknowingly infected.
But who donates blood? According to the Red Cross, only 3 out of 100 of Americans donate. And this 3% is not representative of the population as a whole.
Yes, blood donors come from all races, ages, political affiliations, and economic situations. But they have one thing in common, they are motivated by altruism or a belief that it is in the common good that they donate. They donate because it is the “right thing to do”.
And let’s be practical here for a moment. The type of person who donates blood is not generally the type of person who is irresponsible. If you are a ‘give blood’ type of gay man, you are probably also a ‘get tested’ type of gay man.
So the only unaware HIV-positive infected gay men who are likely to be prevented from donating are those who have good reason to believe (falsely) that they are HIV-negative. That’s not a very big demographic.
3. The FDA does not exclude other demographics who are infected at higher rates than the population at large. For example, over half of all new HIV infections detected in 2007 were in African Americans. While many of those infected are also MSM (men who have sex with men, a term used by the infectious disease community), many are heterosexual. Over 60% of women with AIDS are black. (AVERT)
The estimated lifetime risk of becoming infected with HIV is 1 in 16 for black males, and 1 in 30 for black females, a far higher risk than for white males (1 in 104) and white females (1 in 588).
There are many reasons for this (and for godsake let’s allocate more resources to stemming this trend) and I’m not trying to make comparisons or demonize anyone. But it does demonstrate that the FDA’s banning policies seem inconsistent.
The screening does seek to eliminate those women who might have had sex with a MSM or intravenous drug user in the recent past, but it does not issue a blanket ban based on race (nor should it). However, the “ever had sex at any time in your friggin’ life” definition effectively serves as a ban based on orientation.
So while the FDA does not say that the President of the United States is banned from blood donation based on his ethnicity, it does prohibit donation by Rep. Barney Frank.
4. Not all gay men are equally at risk. Homosexual activity does not create HIV. It is a virus, not a consequence of specific sexual acts. Only about 12% of gay men are infected with the HIV virus.
Yet the FDA treats my friends, a couple in their 40’s who met in high school and have been together ever since, the same as it does some gay man who is single and has an active and diverse sex life. Ironically (and amusingly) it considers ex-gays like Alan Chambers to be no less of a risk than the man whose fetish is to be the recipient in unprotected anal sex.
The FDA clumps gay men into a single demographic and assumes that all gay men are at a higher risk than all heterosexuals.
While statistics indicate a rising infection rate among young heterosexual women, their overall rate of HIV infection remains much lower than in men who have sex with other men.
But clumping in this manner is a foolish and rash policy. Contamination is more likely to come from a young single heterosexual woman who relies on the pill than it is from a gay man in a committed relationship who uses condoms regularly.
5. While the ban on gay men donating does not – in my opinion, as discussed in the points above – serve to diminish much risk of contaminating the blood supply with the HIV virus, it is quite effective at something else: labeling all gay people as dirty and diseased.
This universal ban says, in effect, that all gay men are suspect, a cause of concern, human rats carrying contagion. It feeds the myth that gay equals AIDS and lends credence to the anti-gay activists who market in fear and animus.
But is lifting the ban the answer?
I would argue that a full lifting of the ban is not a wise decision. That would increase – at least in some tiny measure – the risk of taint to the blood pool. Rather, I would advise to change the policy in a way that not only increases the blood supply and to reduces stigma but which also could serve an additional medical function.
Obviously the screening questions need to eliminate the risk of undetected recent infections. But such risks should be based on actual behavior based risk, not on stereotyping of communities. This may even serve to reduce the risk of accidental taint from gay men who ignore the current policy as being nothing more than bias.
Science-based periods of either long-term monogamy or sexual abstinence would likely be respected as reasonable and appropriate. Few gay men would argue that every gay man, regardless of sexual history or responsibility, should donate blood.
And revising the rules for donation to match the requests of the Red Cross would certainly be better than the current policy. But I recommend a different approach.
I recommend that all persons who have any risk of HIV transmission – be they gay men, single heterosexuals, or anyone else who could be at risk – be required to take an HIV test as a step in the donation process. Those persons who tested negative and who had no sexual contact for the previous six months (or whatever restrictions are reasonable) could be treated as acceptable donors. The oral swab tests are non-intrusive, give a response in 20 minutes, and are more than 99% accurate.
The current controls over the blood supply do an amazing job at detecting and removing infected blood. But implementing a screening method that is based on measurability rather than voluntary deferral would effectively eliminate unknown carriers, gay or otherwise.
And it would also reach a population of potentially at-risk citizens who might otherwise go undetected.
The single largest contributor to the spread of HIV is unknown infection. Granted, as I discussed above, those gay men who are most likely to donate blood are also among those most likely to be tested regularly. But HIV testing at a blood donation site could provide access and a safe friendly environment for non-gay people who might be a bit intimidated or uncomfortable asking their doctor or going to the testing center in the gay part of town.
Latest Posts
Featured Reports
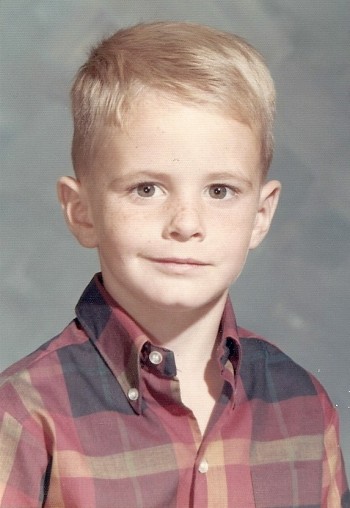 In this original BTB Investigation, we unveil the tragic story of Kirk Murphy, a four-year-old boy who was treated for “cross-gender disturbance” in 1970 by a young grad student by the name of George Rekers. This story is a stark reminder that there are severe and damaging consequences when therapists try to ensure that boys will be boys.
In this original BTB Investigation, we unveil the tragic story of Kirk Murphy, a four-year-old boy who was treated for “cross-gender disturbance” in 1970 by a young grad student by the name of George Rekers. This story is a stark reminder that there are severe and damaging consequences when therapists try to ensure that boys will be boys.
When we first reported on three American anti-gay activists traveling to Kampala for a three-day conference, we had no idea that it would be the first report of a long string of events leading to a proposal to institute the death penalty for LGBT people. But that is exactly what happened. In this report, we review our collection of more than 500 posts to tell the story of one nation’s embrace of hatred toward gay people. This report will be updated continuously as events continue to unfold. Check here for the latest updates.
In 2005, the Southern Poverty Law Center wrote that “[Paul] Cameron’s ‘science’ echoes Nazi Germany.” What the SPLC didn”t know was Cameron doesn’t just “echo” Nazi Germany. He quoted extensively from one of the Final Solution’s architects. This puts his fascination with quarantines, mandatory tattoos, and extermination being a “plausible idea” in a whole new and deeply disturbing light.
On February 10, I attended an all-day “Love Won Out” ex-gay conference in Phoenix, put on by Focus on the Family and Exodus International. In this series of reports, I talk about what I learned there: the people who go to these conferences, the things that they hear, and what this all means for them, their families and for the rest of us.
Prologue: Why I Went To “Love Won Out”
Part 1: What’s Love Got To Do With It?
Part 2: Parents Struggle With “No Exceptions”
Part 3: A Whole New Dialect
Part 4: It Depends On How The Meaning of the Word "Change" Changes
Part 5: A Candid Explanation For "Change"
 At last, the truth can now be told.
At last, the truth can now be told.
Using the same research methods employed by most anti-gay political pressure groups, we examine the statistics and the case studies that dispel many of the myths about heterosexuality. Download your copy today!
And don‘t miss our companion report, How To Write An Anti-Gay Tract In Fifteen Easy Steps.
 Anti-gay activists often charge that gay men and women pose a threat to children. In this report, we explore the supposed connection between homosexuality and child sexual abuse, the conclusions reached by the most knowledgeable professionals in the field, and how anti-gay activists continue to ignore their findings. This has tremendous consequences, not just for gay men and women, but more importantly for the safety of all our children.
Anti-gay activists often charge that gay men and women pose a threat to children. In this report, we explore the supposed connection between homosexuality and child sexual abuse, the conclusions reached by the most knowledgeable professionals in the field, and how anti-gay activists continue to ignore their findings. This has tremendous consequences, not just for gay men and women, but more importantly for the safety of all our children.
Anti-gay activists often cite the “Dutch Study” to claim that gay unions last only about 1½ years and that the these men have an average of eight additional partners per year outside of their steady relationship. In this report, we will take you step by step into the study to see whether the claims are true.
Tony Perkins’ Family Research Council submitted an Amicus Brief to the Maryland Court of Appeals as that court prepared to consider the issue of gay marriage. We examine just one small section of that brief to reveal the junk science and fraudulent claims of the Family “Research” Council.
 The FBI’s annual Hate Crime Statistics aren’t as complete as they ought to be, and their report for 2004 was no exception. In fact, their most recent report has quite a few glaring holes. Holes big enough for Daniel Fetty to fall through.
The FBI’s annual Hate Crime Statistics aren’t as complete as they ought to be, and their report for 2004 was no exception. In fact, their most recent report has quite a few glaring holes. Holes big enough for Daniel Fetty to fall through.
CPT_Doom
March 8th, 2010
The FDA ban applies to more than blood donations, it applies to all tissue donation. Which means if my sister needs a kidney, I can’t give her one, even if she wanted it. If one of her kids needed a bone marrow donation, Uncle Bill is too dirty to help. If I die tomorrow, all my organs will die with me.
There is another impact of the ban. When I was deeply in the closet, I continued to donate, even though I had certainly had (very rare) sex with other men. I could not admit this, even on a form, and thought of my continuing blood donation as a means of “proving” that I wasn’t really gay. The irony is that once I came out I stopped donating (please note, I’m HIV- to this day, 10 years later), even though I was a 3-gallon donor and am CMV- as well (a very rare occurance in anyone over 25). The Red Cross was practically begging for my blood because I am one of the few who could donate to those with compromised immune systems.
daftpunkydavid
March 8th, 2010
from a public health perspective, i thought the fda’s answer was pretty sound. it’s always safer to err on the side of caution. being hiv+, though not a death sentence, can be lived as a serious condition. related tissue transplant questions also arise.
the problem is, as you note, this ban is over-inclusive (all males who have ever had sex with another man since 1977 are banned) and inconsistent all at the same time (other groups that are banned are banned based on behavior, not identity; and other identity groups that overlap with “risky” behavior groups are not banned outright).
moreover, since these decisions are theoretically based on hard evidence, it is going to be difficult to prove that lifting this ban (yet another one to lift) won’t have a negative impact on the safety of the blood supply (geez, aren’t the arguments similar ?!). i say this because there are only a handful of countries that don’t flat out ban men who have ever had sex with at least one other man (russia comes to mind). but i don’t know whether those countries have monitored or studied the results of lifting the ban.
i doubt that such studies would show an increased contamination. indeed with the proper screening protocol, and if they already use rt-pcr, more healthy donors would be able to give their blood, and more donors with risky behavior could be turned down, so in all the process would be safer. no doubt there are people at the fda that share these thoughts.
Elizabeth Casswell
March 8th, 2010
Excellent article. Thank you!
Burr
March 8th, 2010
There’s another inconsistency in their deferrals. If your sexual contact with another man was non-consensual, your deferral is only one year as opposed to indefinite if it was consensual. That makes no sense at all.
The questionnaire should be changed to specify unprotected sexual contact outside of a monogamous relationship. That is the only scientifically valid question, not breaking it down into specifics and caving to bias.
Another thing is this question causes confusion for transgendered individuals. Do they answer as a man or a woman? It can be quite embarrassing and unnecessary even if the context makes that decision obvious.
In the end the questionnaire is relatively pointless and only causes confusion and frustration in potential donors. HIV testing has a false negative rate of 1 in 2 million. HIV transmission from donated blood is exceedingly rare and it has nothing to do with the questionnaire as almost every case of transmission has come from a heterosexual that genuinely didn’t know they were infected.
Another thing, it’s against the law to knowingly lie on the questionnaire about your HIV status, so only a reckless criminal would attempt that.
Burr
March 8th, 2010
When I mention this policy to some of my heterosexual friends and peers, it actually turns them off to donating blood, which is terrible and I try to tell them their blood is still needed and not to let politics get in the way. So to a certain extent it’s really bad for PR as well..
Pender
March 8th, 2010
Burr: your point about non-consensual sex with another man is perfect, and proves all by itself that the policy is not about screening for male sexual contact but rather screening for gay men.
I wish I could corner an FDA policymaker and pose the following:
Suppose a man gets tested for HIV twice, spaced six months apart, and tests negative both times. Suppose he has had sex with only one other man since the first test, and that the other man has had sex only with him during the same time, and that the other man has taken the same tests on the same dates with the same results. Suppose he brings copies of his test results with him to the test center and affirms on the form that he has met all of these guidelines. Suppose you let that man donate blood. Realistically, how much marginal HIV risk would that man bring to the blood pool compared to your average donor?
This policy isn’t about saving lives; it’s about clinging to an age-old slander that gay men are intrinsically pestilent. It’s somewhat understandable why health care workers might cling to that slander, especially if they were active in the health care industry during the ravages of the AIDS crisis, but it’s not evidence-based, despite their protestations, and it’s not justifiable.
David C.
March 8th, 2010
There is a tangential issue here: the available transfusable blood supply is usually limited to days or a very few weeks. We are only one major disaster (such as an earthquake) away from a regional shortage of blood.
As Timothy points out, only about 3% of Americans donate blood. Out-dated and bias-driven prohibitions on the donation of blood by otherwise healthy individuals presents its own risks. If all donated blood is tested, and reasonable deferral periods applied as a function of behavior, the net effect (of diseased donors) on the blood supply would not be measurable—a sudden shortage induced by a large disaster will claim far more lives.
There are also deeper concerns.
The continued ban on gay blood donors is bias driven, plain and simple. That bias may enjoy some science-based justification, but it is indeed tenuous and worthy of wider debate both within the scientific community and society.
The suggestion to allow, perhaps even require an oral HIV antibody test at the time of donation for certain sub-populations of donors seems more scientifically sound than simply concluding that among (the sampled population of) gay men
somehow suggests that truthful answers to a questionnaire are going to protect the nations blood supply from contamination with HIV. Since gay men have been prohibited from donating blood for decades, these statistics seem at least superficially suspect.
While science may be involved, I suspect that politics (and all that comes with it) has a lot more to do with the decision of the FDA.
werdna
March 9th, 2010
Timothy, this is a thoughtful post with a level-headed take on the issue. The safety of gay blood donation can be a challenge to discuss sensibly, sitting as it does on the fraught intersection of demography and bigotry.
The only real quibble I have is regarding your notion of administering a rapid HIV-antibody test at blood donation sites. I don’t think such a proposal would increase the effectiveness of the blood screening process, but it would add a number of potential problems.
All donated blood in the US is already tested for the presence of HIV antibodies. Testing donors before they donate won’t change the efficacy of this technical screening–it won’t make the blood supply any more or less safe. It will, however, add costs to the donation process and significantly increase the amount of time required for some individuals to donate blood.
Furthermore, the Red Cross already notifies donors whose blood tests positive. This is the case not just for HIV but for other blood-born pathogens that the blood is tested for (syphilis, hepatitis, etc.). Because this is done outside of the donation context it’s not necessary to have staff who are trained to deliver these results on hand at all times. If rapid testing is given at the time of donation it’ll be necessary to have such a person available at all donation sites. You won’t increase the number of people who know that they are HIV+ (because donors who test positive are already being notified), but you will make the entire donation process more expensive and cumbersome.
On top of that, confidentiality is a huge concern. Not only for people who test positive (though this is important) but for the individuals who receive the HIV-antibody test as well. Given the semi-public context of many blood donation sites (imagine an office or campus blood drive) dividing donors into groups of those who are determined to be “clean” and those who are potentially risky (i.e., donors who are being tested) is stigmatizing. How could this be managed in such a way as to not make people wonder about which risk factors the separately-tested individuals might have?
The current system allows individuals who know that their blood should not be used to confidentially identify themselves. This avoids producing public stigma (“why wouldn’t they let you donate blood with the rest of us, Bruce?”), and doesn’t require any additional equipment, skills or time. Any new proposals should emulate the elegance of that example.
Getting people to donate blood is hard enough already. The Red Cross does all it can to streamline the process while maintaining strict safety controls. The technical aspect of screening donated blood (antibody testing) is already as effective as it can be. The issue now is tweaking the social elements: how individuals are determined to be eligible to donate or not, how risks are discerned and measured. Adding a procedure that produces no technical advantage but incurs so many costs and complications just doesn’t seem like a good idea.
Burr
March 9th, 2010
werdna is absolutely correct. I wanted to mention something about rapid testing and forgot, but he covered it far better than I could have.
Though I’d add that all blood collectors do what the Red Cross does. It would be an even larger burden for the smaller, regional ones.
Fred in the UK
March 9th, 2010
I fully agree that the policies on gay men donating blood in the US, the UK and elsewhere are irrational. Personally, I don’t feel at all strongly about it, depending on the exact terms of what would be the ‘correct policy’ either it doesn’t effect me (I would still be barred, but by a rational policy) or it saves me from the obligation of actually giving blood myself. I fully realise that I am very much in the minority among gay men here. I would be very grateful if someone who feels strongly on the issue could explain why they feel strongly?
Burr
March 9th, 2010
I feel strongly about it because it has an adverse effect on our blood supply both directly (by disqualifying perfectly valid donor candidates) and indirectly (by confusing and discouraging other potential donors, including heterosexual ones). We can’t afford to turn away anyone as it is.. To me it’s as much (or even more) about pragmatism than idealism.
Burr
March 9th, 2010
The questionnaire also asks women if they had sexual contact with a man who has had sexual contact with another man and defers them as a result. How in the world is a woman supposed to answer that question with absolute certainty?
Besides, the nation’s blood centers are fully behind changing the policy. I think it’s safe to defer to the REAL experts on this one, not the FDA, which has a far worse record of poor decisions leading to unnecessary deaths than the blood banks.
Leave A Comment