Box Turtle Bulletin
 News and commentary about the anti-gay lobby
News and commentary about the anti-gay lobby News and commentary about the anti-gay lobby
News and commentary about the anti-gay lobbyThis commentary is the opinion of the author and may not necessarily reflect that of other authors at Box Turtle Bulletin
March 31st, 2010
It has long been known that HIV and AIDS in the United States is not experienced proportionately across racial demographics. About 42% of all cumulative AIDS cases, and over 50% of new HIV infections are in African Americans, even though they only comprises about 14% of the population.
And results released last week about a survey of gay men in Washington, D.C. confirm the pattern. While the study found that 14% of the sample of gay men are HIV positive, this was not uniformly distributed.
Men of color who were 30 years or older had the highest rate, more than twice the overall HIV positivity rate. By race and all ages, over a quarter (25%) of black men who participated in the study were HIV positive, more than any other racial group. Over 10% of men who identified as multirace (11%) and other (10%) were HIV positive and 8% of white males who participated in the study were HIV positive.
In fact, this difference was most notable in participants under 30. While 12.2% of young men of color were HIV infected, “of the nearly 100 white men younger than 30, none were HIV-positive.”
This disparity is usually discussed, when it is discussed at all, in terms of social or cultural difference (especially by those who are not African-American). Non-equivalent infection rates are “part of the down-low” or “the result of homophobia in the black community” or “resultant from a lack of self-worth” or some other culture based phenomenon that hints at irresponsible behavior or an inadequate appreciation for safer sex rules.
I do not doubt that there are some social factors (discrimination, economic inequalities, social position, or even media representation) that do contribute to the prevalence of HIV in Black America. But something in this study caught my attention.
Over 40% of men did not use a condom at last sex, though men of color used condoms nearly twice as much as white men.
Younger men who have receptive anal sex (“bottoms”) and older men who have insertive anal sex (“tops”) were less likely to use condoms.
But if black men were twice as likely to use a condom, then how exactly is it that they were more likely to seroconvert?
One explanation that has been bandied about is that because the pool of black men who sleep with black men is already disproportionately infected. Therefore, because there is an increased risk of contact with infected sex partners it raises the likelihood of higher infection rates.
But that doesn’t seem to be evidenced by the results of this study.
The research allows us to compare those who were already aware of their HIV status to those who were newly infected, by race. Assuming that black men were adhering more closely to safe-sex guidelines, this should have been reflected in the ratios. But newly infected men were even more disproportionately men of color than were those already detected.
This seems contradictory to the notion that black men use condoms at higher rates than whites. So perhaps something else is going on. Perhaps there is something other than behavior that is contributing to the disparity.
We know that some communities inherently carry higher risk of certain diseases while others are fairly immune. Tay-Sacks is more commonly found in Ashkenazi Jews, sickle cell anemia is associated with people with recent ancestry from parts of Africa, the Mediterranean, India and the Middle East, and some Scottish islands have higher incidences of color blindness. These are all the results of inherited genes.
So it should not surprise us that various communities may have inherited genetic susceptibilities or immunities that greatly impact the extent to which any individual in that community is at risk for HIV transmission. And, indeed, research does seem to suggest that not all ancestor-location based gene pools respond to potential infection in the same way.
Some people seem to have inherited a resistance to HIV, effectively leaving them immune from infection.
Genetic resistance to AIDS works in different ways and appears in different ethnic groups. The most powerful form of resistance, caused by a genetic defect, is limited to people with European or Central Asian heritage. An estimated 1 percent of people descended from Northern Europeans are virtually immune to AIDS infection, with Swedes the most likely to be protected. One theory suggests that the mutation developed in Scandinavia and moved southward with Viking raiders.
Similarly, it appears that some communities have inherited ahigher susceptibility to HIV infection.
New research shows Africans and people of African descent could be up to 40 percent more likely to get HIV, the virus that causes AIDS, than people of other races.
This appears to be related to the Duffy antigen, a protein on the surface of red blood cells, which plays are role in defense against malaria. This trait appears to be present in over 90% of black Africans and about 70% of African Americans.
Indeed, as I looked for further discussion on the subject of gene-linked susceptibility, it seems that the community of scientists looking for transmission patterns, infection factors, and treatment possibilities share an assumption that genes play a significant role, and one we do not yet fully understand. And even within specific racial groups, some genetic families may be far more susceptible than others.
But this contributing factor seems to be, to a great extent, outside of common knowledge. Even most gay men – including those I know of African descent – seem not be be aware of genetic factors that contribute to increased or decreased infection risk.
And this troubles me. I believe that this is of such significance that it should be emphasized, particularly among those who may have inherited a higher possibility of infection.
As I see it, there are several reasons why an increased understanding of possible racial group or family genetic traits should be part of our consciousness.
First, if African-Americans are not aware of increased risk, they cannot be prepared. And as we learn more about subgroups or families, individuals of all races can take steps to define “safe sex” in more specialized ways. As unfair as such knowledge may seem, knowing that you can’t live by the same standards as everyone else may have life impacting importance for some individuals.
It’s all fine and good to say “always be safe”, but everyone knows someone who slipped up and ended up okay. But if some individuals have inherited higher risk , they need to know that the answer to “what are the odds” is “much higher for me so I don’t dare risk it… ever.”
Second, a different response in one’s body to the presence of HIV should be reflected in treatment and management. It would be foolish not to test to determine whether some treatment protocols were more or less effective based on inherited factors.
Our nation has a history of medical research that assumes that everyone is a white male, and a fairly interchangeable one at that. But if different protocols are more effective for those of African descent, or for others with specific genetic heritage, it would be immoral not to test for such differences and instead rely on, “this is what works for wealthy white men in West Hollywood”.
Third, vaccines under testing should be studied for whether race or inherited attributes impacts effectiveness. I am troubled by the possibility that some vaccines which were discarded as ineffective in some trials may have been very effective in a different demographic.
But I think we need to approach this with sensitivity. HIV/AIDS has a history of blame and stigma; And any discussion which seeks to assign blame or which seeks to make HIV a “black disease” will do more harm than good.
Additionally, we should remember that individuals are, above all else, individual. We should not make assumptions or assign stereotypes.
Instead, we need to focus research and funding, coordinate outreach and education, and for once talk about the impact of HIV on the African American community without hinting that the phenomenon can be explained in terms of behavior.
And in the meanwhile, let’s find a way to be part of the solution. You can contribute to HIV/AIDS prevention efforts that specifically target the African-American community:
National Black Justice Coalition
BlackAIDS.org
(my appreciation to those who read the draft and provided some insight and suggested revision)
Latest Posts
Featured Reports
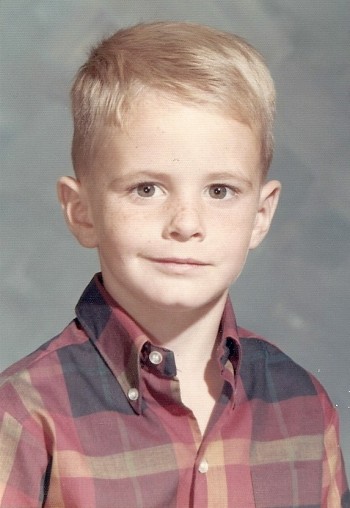 In this original BTB Investigation, we unveil the tragic story of Kirk Murphy, a four-year-old boy who was treated for “cross-gender disturbance” in 1970 by a young grad student by the name of George Rekers. This story is a stark reminder that there are severe and damaging consequences when therapists try to ensure that boys will be boys.
In this original BTB Investigation, we unveil the tragic story of Kirk Murphy, a four-year-old boy who was treated for “cross-gender disturbance” in 1970 by a young grad student by the name of George Rekers. This story is a stark reminder that there are severe and damaging consequences when therapists try to ensure that boys will be boys.
When we first reported on three American anti-gay activists traveling to Kampala for a three-day conference, we had no idea that it would be the first report of a long string of events leading to a proposal to institute the death penalty for LGBT people. But that is exactly what happened. In this report, we review our collection of more than 500 posts to tell the story of one nation’s embrace of hatred toward gay people. This report will be updated continuously as events continue to unfold. Check here for the latest updates.
In 2005, the Southern Poverty Law Center wrote that “[Paul] Cameron’s ‘science’ echoes Nazi Germany.” What the SPLC didn”t know was Cameron doesn’t just “echo” Nazi Germany. He quoted extensively from one of the Final Solution’s architects. This puts his fascination with quarantines, mandatory tattoos, and extermination being a “plausible idea” in a whole new and deeply disturbing light.
On February 10, I attended an all-day “Love Won Out” ex-gay conference in Phoenix, put on by Focus on the Family and Exodus International. In this series of reports, I talk about what I learned there: the people who go to these conferences, the things that they hear, and what this all means for them, their families and for the rest of us.
Prologue: Why I Went To “Love Won Out”
Part 1: What’s Love Got To Do With It?
Part 2: Parents Struggle With “No Exceptions”
Part 3: A Whole New Dialect
Part 4: It Depends On How The Meaning of the Word "Change" Changes
Part 5: A Candid Explanation For "Change"
 At last, the truth can now be told.
At last, the truth can now be told.
Using the same research methods employed by most anti-gay political pressure groups, we examine the statistics and the case studies that dispel many of the myths about heterosexuality. Download your copy today!
And don‘t miss our companion report, How To Write An Anti-Gay Tract In Fifteen Easy Steps.
 Anti-gay activists often charge that gay men and women pose a threat to children. In this report, we explore the supposed connection between homosexuality and child sexual abuse, the conclusions reached by the most knowledgeable professionals in the field, and how anti-gay activists continue to ignore their findings. This has tremendous consequences, not just for gay men and women, but more importantly for the safety of all our children.
Anti-gay activists often charge that gay men and women pose a threat to children. In this report, we explore the supposed connection between homosexuality and child sexual abuse, the conclusions reached by the most knowledgeable professionals in the field, and how anti-gay activists continue to ignore their findings. This has tremendous consequences, not just for gay men and women, but more importantly for the safety of all our children.
Anti-gay activists often cite the “Dutch Study” to claim that gay unions last only about 1½ years and that the these men have an average of eight additional partners per year outside of their steady relationship. In this report, we will take you step by step into the study to see whether the claims are true.
Tony Perkins’ Family Research Council submitted an Amicus Brief to the Maryland Court of Appeals as that court prepared to consider the issue of gay marriage. We examine just one small section of that brief to reveal the junk science and fraudulent claims of the Family “Research” Council.
 The FBI’s annual Hate Crime Statistics aren’t as complete as they ought to be, and their report for 2004 was no exception. In fact, their most recent report has quite a few glaring holes. Holes big enough for Daniel Fetty to fall through.
The FBI’s annual Hate Crime Statistics aren’t as complete as they ought to be, and their report for 2004 was no exception. In fact, their most recent report has quite a few glaring holes. Holes big enough for Daniel Fetty to fall through.
David
March 31st, 2010
Income may be a factor as well – not all condoms are equal, cheaper brands tend to be more likely to fai. And it is possible to sero-convert having used condoms for every sexual encounter – through condom failure.
Since race and income still correlate strongly in the U.S., its worth considering.
Additionally, HIV Awareness/safer sex campaigns have tended to focus on men of European descent more than African-American men for much of the history of the epidemic. The subliminal messages given 10 or more years ago could easily be bearing fruit today.
And lastly, safer-sex education was significantly hindered by right-wing political efforts for more than a decade, and the effects of that obstructionism may have had a income level related distribution as well.
Of course, since the virus had decades to develop in Africa before it was even identified, it may simply be better adapted to people with a defense against malaria.
Pender
March 31st, 2010
Some people will probably lie about having used a condom. Doesn’t seem far-fetched that propensity to lie about that could inversely correlate with education, which unfortunately inversely correlates with being black.
Not saying it’s not possible that there is a genetic susceptibility at work here, but it seems to me that surveys dealing with issues as fraught as safe sex, gay sex and HIV are going to be plagued with data reliability issues.
anteros
March 31st, 2010
condom use does not necessarily mean safer sex. not everybody gets all the info they need on safer sex, especially groups that generally suffer more stigma and discrimination than others. i wouldnt be surprised if many of those who claimed they used condoms were making serious but common mistakes that many people dont even consider… exposing condoms to unfavorable and damaging conditions by keeping them in back pockets or in cars, improper application, wearing two or more condoms, not using lube for anal sex, using inappropriate substances in place of water-based lube, careless withdrawal, improper disposal… effective condom use (especially for anal sex) is actually a more delicate art than what is suggested by most safer sex messages, “always use a condom”, “no glove no love”, …safer sex messages in hip hop songs are woefully inadequate for gay men. sadly, such dangerously inadequate “hetero-centric” safer sex messages are more likely to dominate in communities that are more homophobic or less open about gay sex.
that said, the solution may not be as simple as aggressively marketing “homo-centric” safer sex messages for the black LGBT community. i agree… there must be something else going on. whether it’s a genetic thing or not, more vulnerable groups ought to be made more aware of such vulnerabilities. perhaps that should be included in more homo-centric safer sex campaigns in the black LGBT community. it’s a very sensitive issue, but it’s a serious matter requiring urgent attention that shouldn’t be bogged down by political correctness.
foxx
April 1st, 2010
Wake the hell up “Amerikkka”!!! AIDS/HIV is a “man ~ made” disease. It was created by a scientist in a Government Lab at Ft. Detrick, Maryland!!! It is being used as a “WMD” to commit “Genocide” against the Black Race here in Amerikkka and Africa!!! BTW they already have a “cure/vaccine” for AIDS/HIV, but it is “NOT” available to the general public, it’s “ONLY” available to the “Elite.” There is “no money” to be made in the “cure,” the money is being made by selling the expensive medicine!!! DUH!!!
foxx
April 1st, 2010
[Foxx posted a lengthy article cut from another site. For several reasons, we do not host other people’s material. If you wish to read the article you may do so here.]
justsearching
April 1st, 2010
Yup Fox.
1. Gather up a whole bunch of sketchy bits of information (the more the better)
2. Make wild conclusions based on said information
3. Make further wild conclusions based on the conclusions made in #2
I think I prefer Timothy’s approach.
foxx
April 1st, 2010
[Foxx posted a lengthy article cut from another site. For several reasons, we do not host other people’s material. If you wish to read the article you may do so here.]
foxx
April 1st, 2010
RE: justsearching
April 1st, 2010 | LINK
Yup Fox.
1. Gather up a whole bunch of sketchy bits of information (the more the better)
2. Make wild conclusions based on said information
3. Make further wild conclusions based on the conclusions made in #2
I think I prefer Timothy’s approach.
I have provided the “TRUTH” and good information with Links, if you choose not to believe me then it’s your “loss.” None are so “blind,” as those who will “not” see!!! You probabaly think the Tuskegee Experiment was a “hoax” too!!!
Geekydee
April 1st, 2010
@foxx
thank you for the very interesting article. I believe it does show a definite correlation with stated facts that have been found. Also, I find the mention of this in the wiki article on visna (which is cited): “The susceptibility of Maedi-Visna infection varies across sheep breeds, with coarse-wool breeds apparently more susceptible than fine-wool sheep” to be somewhat disturbing; I need to find someone with access to the source at ScienceDirect. Be that as it may, I found it interesting in that I have no immune system due to genetic quirk (CVID from Black Forest region ancestors) and I am thoroughly intrigued by all this. Again, thank you for the highly informative article :)
anteros
April 1st, 2010
foxx:
that sounds like a recipe for bitterness… and apathy.
if it were a man-made virus, or if it originated in Africa (i’m not convinced on any origin theories)… does that mean we can’t beat the virus?
forget stuff that induces apathy.
think of solutions… research… education… spread awareness… personal and collective agency… empowerment… anything that can make a difference or help people in anyway. it’s already being done, but more needs to be done… it’s not over yet.
i’m not suggesting that you have never done anything helpful. all i’m saying is… apathy is one of the virus’ allies… and theories that induce apathy, whether factual or not, ought to be shelved in favor of more solution-oriented discussions. that’s all.
Mark F.
April 1st, 2010
Interesting topic.
I think the safer sex message to ALL gay men has to be this:
Seriously consider abstaining ~totally~ from anal sex, unless you are with a monogamous partner you can trust.
99.9 % of gay men get HIV from anal sex.
If you must have anal sex, use a condom every time. Or try a sex toy.
anteros
April 1st, 2010
i’m sorry but “always use a condom” is not an adequate safer sex message for men who have sex with men, and people need to understand why. please check out these resources:
http://www.playnice.me
http://www.health4men.co.za
i hate to bring this up, but isn’t there a disproportionate number of black males who are or have been incarcerated? i’m not sure how much safe sex is preached, facilitated or practiced in jail, but i’m wondering… aren’t infection rates higher among men who have sex with men in jail? …considering prison rape, including gang rape? does that have an effect on overall infection rates among black men who have sex with men? if it does, is anybody doing anything about it, at all?
Jim Burroway
April 1st, 2010
I have removed Foxx’s much longer comment. We don’t host conspiracy theories about AIDS being “man made” and the result of medical experiments designed to “annihilate, decimate and castrate African, Hispanic and Asian peoples under the rubric of European supremacy.” While Foxx sites “sources,” the sources he cites — particularly the so-called “Strecker Memorandum,” — haven’t even the remotest credibility within the scientific community, nor is there a shred of evidence in peer-reviewed publications to support such wild accusations.
The facts surrounding the unconscionable Tuskogee experiments, on the other hand, are widely verifiable through multiple reputable sources, not the least of which the declassified medical records of the men and women from whom treatment was withheld.
Hosting this nonsense is comparable to lending credence that the world if flat or the moon really is made of cream cheese. Or that Paul Cameron is a researcher. We won’t do that.
Regan DuCasse
April 1st, 2010
Outstanding analysis. I’ve participated in the Black Women’s Health Study for over ten years. Their questionnaire is concerned with STD’s, most importantly HIV/AIDS and condom use.
Black women in America comprise a comparable high risk group to that of gay men.
Unfortunately, a strong stereotype that influenced the information track was that ONLY gay men got HIV. Then the OTHER was that it was gay men having sex with women that introduced the virus to hetero black women.
There are several publications of interest to black women, and they have done much to dispel or correct previous misinformation about how the disease tracked into the black community.
Essentially, the truth is, black hetero men who don’t or refuse to use condoms have been the culprits all along. Black men especially, in some communities, have multiple partners within short periods of time. Especially in lower income neighborhoods where there might be more resistance to, or less access also to information and preventive measures.
It’s a cultural factor, a kind of macho attitude that makes some black men refuse to use condoms and live in a state of denial. Denial of personal responsibility to prevention of disease or pregnancy. Invariably they will blame the woman for whatever outcome occurs.
It’s been most unfortunate that black gay males and black hetero females are the most isolated from social protection, inclusion and economic empowerment.
However, if there IS a kind of genetic factor that makes HIV more stubborn and resistant to medical intervention, it’s worth researching.
I have systemic lupus. A genetic auto immune disorder that disproportionately affects WOMEN, and at another level, disproportionately affects black women.
It’s fair to speculate and respond to such a possibility.
But as long as those most vulnerable are also the most dislocated from medical and educational research and access, then a comprehensive result will be elusive.
David
April 1st, 2010
For anyone who wasted their time with Foxx’s link:
“However, a study in 200815 dated the origin of HIV to between 1884 and 1924, much earlier than previous estimates. The researchers compared the viral sequence from 1959 (the oldest known HIV-1 specimen) to the newly discovered sequence from 1960. They found a significant genetic difference between them, demonstrating diversification of HIV-1 occurred long before the AIDS pandemic was recognised.”
http://www.avert.org/origin-aids-hiv.htm
Foxx, it is entirely inappropriate to make April Fools day jokes about HIV/AIDS, and that is the best your posts can be.
Regan DuCasse
April 1st, 2010
Stigma, has no place in a discussion or among those seriously committed to preventing or eradicating a disease like HIV. Or herpes for that matter.
I’ve noticed that those who are anti gay, cannot discuss the full spectrum of history and pandemics in it’s proper context.
They seem flummoxed when I mention that syphilis was the AIDS of it’s own time and was with us for CENTURIES before a cure was developed in the last century.
Rather than posit the discussion in terms of FIGHTING THE DISEASE, through funding of research, education, scholarships for the most talented bio medical professionals and so on: they’d rather fight the PEOPLE who are at risk and condemn them to more of the socio/political isolation that increased the pandemic.
Even those people of faith, if I asked them to pray and support that HIV/AIDS goes the way of syphilis and there is a vaccine or cure found, and that human suffering can be relieved only through committed dedication to medical compassion, not discrimination…I might as well have whistled in the wind.
Am I being naive that there SHOULD be a meeting of the minds on this, regardless of being religious or not?
I mean, seriously…what IS the point in dedicating SO much time in making gay people be among the disappeared, instead of an infection that affects EVERYONE?
Is there some Biblical or religious definition for this kind of folly?
Leave A Comment