Box Turtle Bulletin
 News and commentary about the anti-gay lobby
News and commentary about the anti-gay lobby News and commentary about the anti-gay lobby
News and commentary about the anti-gay lobbyJuly 19th, 2012
 The Black AIDS Institute has released a new publication in which they detail the statistics relating to HIV infection within the black gay and bisexual community. But while the report is very grim (and I’ll discuss that separately), Executive Director Phill Wilson said something that surprised me in its forthrightness:
The Black AIDS Institute has released a new publication in which they detail the statistics relating to HIV infection within the black gay and bisexual community. But while the report is very grim (and I’ll discuss that separately), Executive Director Phill Wilson said something that surprised me in its forthrightness:
There is hope, however. New evidence indicates that antiretroviral treatment reduces the odds of HIV transmission by 96%, leading preeminent scientific experts to advise that the tools now exist to end the AIDS epidemic – for all populations, and in all settings.
As I thought about this, I realized that it’s true. We have the technical ability to ensure that the transmission of HIV from infected to uninfected persons stops. Entirely.
The Problem
Currently, nearly all cases of seroconversion are due to sexual activity. And while moralists are correct that “if sex was limited to marriage” the virus would be halted, that is not a realistic plan (or one that is based in finding a way to reduce transmission). And while “everybody must use a condom every time” was for a time the only possible approach, it is evident that it is not and will not be the plan that eliminates transmission.
There are a number of reasons that “condoms every time” fails. Discomfort, inconvenience, the awkwardness of sexual negotiation. But the most significant reason, the single largest contributor to the spread of HIV, is personal ignorance about HIV status.
Sure there are some totally amoral bastards who hide behind “It’s your responsibility to protect yourself and I have no obligation to divulge my status” and a few on the opposite side who find a thrill in the risk of the unknown. But most people who are positive take steps not to pass on the virus and those who are negative do engage in some measures (though not always wise or effective) to minimize exposure, even if that step is limited to asking and placing too much reliance on the answer.
But one thing keeps transmission rates steady or increasing year after year. One thing we can halt: ignorance.
The Solution
The key to stopping HIV is knowledge. The CDC estimates that between a quarter and a third of those who are HIV positive are not aware of their serostatus. And that is a reality that we could end – if we have the resolve to do so.
In British Columbia, officials have announced a new goal and allocated funding for it. (globeandmail)
Saying it is now possible to end HIV/AIDS, medical experts in British Columbia have launched a four-year, $48-million pilot program aimed at detecting and treating the disease faster.
The goal is to test everyone in the province who has ever been sexually active.
The sweeping approach is an attempt to catch the estimated 1 per cent of people who are unaware they are HIV-positive and aren’t taking advantage of an effective treatment program that is available provincially.
This is the right approach and we should find a way to implement it globally.
The Complications
Of course, British Columbia only has 4.4 million people and universal health care so it’s not as easy as insisting that every state, province and nation follow suit. But testing is inexpensive and highly accurate. For less than $20 per person (BC is only spending $10) we could identify nearly every HIV positive person in our city, state, nation.
Even in states and countries in which there is insufficient postconversion medical care, even if this would place a burden of dread on those diagnosed, there would be knowledge. And knowledge would reduce future transmissions. (And surely we care as much about the physical health of the person who would be saved from seroconversion as we do about the mental health of the newly diagnosed.)
But knowledge is not the only key to complete elimination of future transmissions. We also have the tools to stop transmission when knowledge is ignored or when accidents occur.
The Tools
Highly active antiretroviral therapy, or HAART, is a combination of three or four separate drugs that prohibit various steps of HIV replication (what we used to call a “drug cocktail”) and is highly effective. The vast majority of those who consistently use this process reduce replication of the virus within their system to the point where it is “undetectable”. And with the reduction in viral load comes a reduction in transmittablity – possibly to the point where the virus cannot be transmitted through sexual activity.
It is true that many HIV infected people do not have funds – or insurance – to pay for a medicine regimen. But there are programs established which are designed specifically to assist such people and when exact numbers can be provided it will be politically difficult for officials to intentionally deny funding for specific individuals who can be identified.
On the other side of the equation, the Food and Drug Administration has just approved the use of an AIDS drug for preventative measures. Pre-Exposure Prophylaxis (PrEP) is only currently advised for those who are at highest risk (and as yet with unidentified means of paying for such a drug) and we cannot know the extent to which this will diminish transmission, but it could play a significant role if prioritized and adequately funded. This drug can virtually eliminate the ability for HIV to infect the who take it consistently and properly.
Finally, it is now possible to eliminate transmission after “the condom broke”. Those who engage in sexual behavior that is risky have a second chance, an ability to reverse their bad decision (or, as actually does happen, when the condom breaks). Post-Exposure Prophylaxis (PEP), a drug regimen started within 72 hours and taken consistently for a month, has shown high effectivity in prohibiting seroconversion.
But all of this relies on knowledge. You won’t get treatment if you aren’t tested and the likelihood of PEP being utilized is greatly decreased if the insertive partner is unaware of his HIV status. And there will be those who refuse to care for themselves or who lack the structure to commit to a regimen and for whom PrEP, PEP, or retroviral regimen will not be a reality. But they are only one cog in the transmission cycle.
And this is not to suggest that everyone in a serodiscordant relationship or who enjoys frequent sexual diversity should adopt a PrEP regimen. Nor will those who select serosorting or seropositioning likely replace their choices with either drugs or condoms. But these are tools that can be employed.
And using all our tools together – a universal testing strategy combined with treatment for those who are positive, PrEP for those who are either in serodiscordant relationships or whose behavior is at high risk for conversion, and PEP readily and immediately available at every local drugstore (perhaps through 24/7 dial up prescription), all as a supplement to a message of consistent condom use – we could effectively end the transmission of HIV.
The Proposal
I know it sounds like a the final scene of Longtime Companion and a bit too hollywood to be real. After two decades, I’m not sure we believe in happy endings any longer. But it really can happen.
And I have a proposal for how we could roll out a program that could give us that day when HIV transmission is a sad history and not a present reality, and see it in this decade. My idea will not sit easily with some and will run into automatic objections. But I hope that when I present it tomorrow that you’ll give it a fair hearing.
Latest Posts
Featured Reports
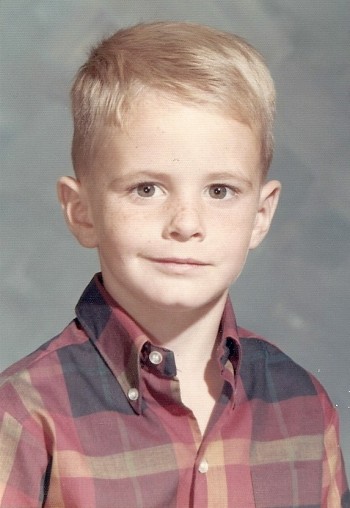 In this original BTB Investigation, we unveil the tragic story of Kirk Murphy, a four-year-old boy who was treated for “cross-gender disturbance” in 1970 by a young grad student by the name of George Rekers. This story is a stark reminder that there are severe and damaging consequences when therapists try to ensure that boys will be boys.
In this original BTB Investigation, we unveil the tragic story of Kirk Murphy, a four-year-old boy who was treated for “cross-gender disturbance” in 1970 by a young grad student by the name of George Rekers. This story is a stark reminder that there are severe and damaging consequences when therapists try to ensure that boys will be boys.
When we first reported on three American anti-gay activists traveling to Kampala for a three-day conference, we had no idea that it would be the first report of a long string of events leading to a proposal to institute the death penalty for LGBT people. But that is exactly what happened. In this report, we review our collection of more than 500 posts to tell the story of one nation’s embrace of hatred toward gay people. This report will be updated continuously as events continue to unfold. Check here for the latest updates.
In 2005, the Southern Poverty Law Center wrote that “[Paul] Cameron’s ‘science’ echoes Nazi Germany.” What the SPLC didn”t know was Cameron doesn’t just “echo” Nazi Germany. He quoted extensively from one of the Final Solution’s architects. This puts his fascination with quarantines, mandatory tattoos, and extermination being a “plausible idea” in a whole new and deeply disturbing light.
On February 10, I attended an all-day “Love Won Out” ex-gay conference in Phoenix, put on by Focus on the Family and Exodus International. In this series of reports, I talk about what I learned there: the people who go to these conferences, the things that they hear, and what this all means for them, their families and for the rest of us.
Prologue: Why I Went To “Love Won Out”
Part 1: What’s Love Got To Do With It?
Part 2: Parents Struggle With “No Exceptions”
Part 3: A Whole New Dialect
Part 4: It Depends On How The Meaning of the Word "Change" Changes
Part 5: A Candid Explanation For "Change"
 At last, the truth can now be told.
At last, the truth can now be told.
Using the same research methods employed by most anti-gay political pressure groups, we examine the statistics and the case studies that dispel many of the myths about heterosexuality. Download your copy today!
And don‘t miss our companion report, How To Write An Anti-Gay Tract In Fifteen Easy Steps.
 Anti-gay activists often charge that gay men and women pose a threat to children. In this report, we explore the supposed connection between homosexuality and child sexual abuse, the conclusions reached by the most knowledgeable professionals in the field, and how anti-gay activists continue to ignore their findings. This has tremendous consequences, not just for gay men and women, but more importantly for the safety of all our children.
Anti-gay activists often charge that gay men and women pose a threat to children. In this report, we explore the supposed connection between homosexuality and child sexual abuse, the conclusions reached by the most knowledgeable professionals in the field, and how anti-gay activists continue to ignore their findings. This has tremendous consequences, not just for gay men and women, but more importantly for the safety of all our children.
Anti-gay activists often cite the “Dutch Study” to claim that gay unions last only about 1½ years and that the these men have an average of eight additional partners per year outside of their steady relationship. In this report, we will take you step by step into the study to see whether the claims are true.
Tony Perkins’ Family Research Council submitted an Amicus Brief to the Maryland Court of Appeals as that court prepared to consider the issue of gay marriage. We examine just one small section of that brief to reveal the junk science and fraudulent claims of the Family “Research” Council.
 The FBI’s annual Hate Crime Statistics aren’t as complete as they ought to be, and their report for 2004 was no exception. In fact, their most recent report has quite a few glaring holes. Holes big enough for Daniel Fetty to fall through.
The FBI’s annual Hate Crime Statistics aren’t as complete as they ought to be, and their report for 2004 was no exception. In fact, their most recent report has quite a few glaring holes. Holes big enough for Daniel Fetty to fall through.
Truthspew
July 20th, 2012
They are damnably close to a vaccine against HIV right this minute. Animal trials are going well and they expect human trials to begin soon.
If it is effective I’d like to see every child vaccinated for it like we vaccinate for MMR, Tdap, etc.
Palmer
July 20th, 2012
Truthspew, we’ve been damnably close to a vaccine for over fifteen years, and every time it turns into another chimera.
DenguyFL
July 20th, 2012
Mr Kincaid, you bring a lot of good points out in this column then you go and undermine your credibility as someone to listen to when you say the following, “You won’t get treatment if you aren’t tested and the likelihood of PEP being utilized is greatly decreased if the insertive partner is unaware of his HIV status.” The insertive partner should be just as concerned if the receptive partner is positive. HIV doesn’t actually care which you are. yes there is a statistical difference in likelihood of transmission but it is not non-existent. It is this type of sentence that creates the myth that only receptive partners are susceptible to HIV transmission.
Please be more careful about this in the future.
Leave A Comment