Box Turtle Bulletin
 News and commentary about the anti-gay lobby
News and commentary about the anti-gay lobby News and commentary about the anti-gay lobby
News and commentary about the anti-gay lobbyDecember 8th, 2012
 Tonight at sundown marks the start of the first day of Hanukkah. The story behind the eight days of Hanukkah is pretty cool: after the forces of Antiochus IV had been driven from the Temple, the Maccabees discovered that all of the ritual olive oil used to light the Temple menorah had been profaned — all except for one container that was still sealed by the High Priest. It had enough oil to keep the menorah lit for only one day, which meant that it would have run out before they could press and prepare more oil in a process that took eight days. But miraculously, that one-day supply lasted all eight days, and the light never went out.
Tonight at sundown marks the start of the first day of Hanukkah. The story behind the eight days of Hanukkah is pretty cool: after the forces of Antiochus IV had been driven from the Temple, the Maccabees discovered that all of the ritual olive oil used to light the Temple menorah had been profaned — all except for one container that was still sealed by the High Priest. It had enough oil to keep the menorah lit for only one day, which meant that it would have run out before they could press and prepare more oil in a process that took eight days. But miraculously, that one-day supply lasted all eight days, and the light never went out.
Cool story. Just about as cool as the Christmas story. And one way you know that its coolness is approaching Christmassy coolness is the way Hanukkah merchandise is becoming just as commercialized and tacky as Christmas tchotchkes (which, by the way, is a really cool Yiddish word). I used to think it looked kinda patronizing whenever we’d walk into a Crate and Barrel festooned with Christmas stuff and see that one tiny little corner set aside for a Hanukkah display. “Oh look,” I’d say to my partner in my best morning television host voice, “and now we have something for our Jewish friends.” But now Hanukkah has gone all steampunk, and that just takes its coolness to a whole ‘nother level.
Of course, the jury still out as to which level that actually is.
Happy Hanukkah!
TODAY’S AGENDA:
Events This Weekend: Mad Bear, Madrid, Spain; Pride Manila, Manila, Philippines.
THIS MONTH IN HISTORY:
Aversion Therapy of Homosexuality: 1969. Doctors had been using painful jolts of electricity to try to torture homosexuality out of people since 1935 (see Mar 15 and Sep 6), and when Behavioral Therapy became one of the more dominant forms of therapy in the 1960’s, gay people were getting shocked right and left. In 1969, The British Journal of Psychiatry published a paper by John Bancroft of Maudsley Hospital, a psychiatric facility in South London, titled “Aversion Therapy of Homosexuality: A Pilot Study of 10 cases.” The purpose of the paper was to provide a longer-term follow-up of the first ten cases of a larger group of 40, with “the minimum follow-up period being one year.”
The treatment went like this: first, the patient’s penis was attached to a sensitive measurement device to detect any changes in its girth. Then:
In method A, the patient was asked to produce erotic homosexual fantasies whilst looking at photographs of males. Painful electric shocks were delivered to his arm whenever an erection developed up to a certain level. (In most cases the level used represented an increase in the circumference of the penis of approximately 0.6 mm. This reflects a change of which the subject is not usually aware but which is reliable and distinguishable from artifact.) Following this initial shock, further shocks were given at 15 second intervals unless the erectile response was falling or was once again below the threshold level. A minimum of 5 shocks was given in any one trial.
If the threshold level of erection was not reached by the end of 5 minutes, the trial was ended and a new trial was started with different photographs. On the average, 12 such trials were given in each session.
In addition each session included two further types of trial; one homosexual trial with no threat of shock, and 3 heterosexual trials when photographs of females were used and the patient encouraged to produce heterosexual fantasies. These heterosexual trials were included for two reasons. Firstly to allow discrimination between homosexual and heterosexual erections and so avoid any suppression of homosexual erections generalizing to both. Secondly it was hoped that either by a practice effect or by an “anxiety relief” effect (due to withdrawal of the threat of shock) the heterosexual responses might be reinforced.
In the last three patients an alternative method was used in the last part of treatment (Method B). In this method, the patient was asked to produce specific homosexual fantasies without the use of photographs, and to signal as soon as he had the image clearly in his mind. He was then shocked. In this second method, therefore the noxious stimulus was not contingent upon the erectile response but upon the fantasy.
Before or after the sessions, the patients were asked to describe any sexual activity they had participated in, as well as their masturbatory fantasies. The answers to those questions determined whether they passed or failed. How very scientific, don’t you think? But what’s most revealing is how Bancroft described the treatment effects for each of the ten patients. Each description is worth looking at:
Patient A: He was a 36 year old artist “of good personality” who , aside from a few dalliances, was “clearly heterosexual in his outlook.” He was married, but had frequent flings on the side. He volunteered for aversion therapy after reading about it in a newspaper article. “After 30 sessions he was initiating homosexual encounters but finding himself impotent. This had never happened before. Treatment was stopped after 45 sessions when he felt he could control the urges.” But on follow-up, he gradually returned “to his previous pattern. He was given a further course of treatment using method B; this gave him greater control but only whilst the treatment was continuing. Three and a half years after treatment homosexual encounters continue but the frequency is less than before treatment, the urges are less strong, and he is getting less pleasure from them.”
Patient B: A 28-year-old postal worker who “came for treatment because he was frightened by a police charge.” After 21 sessions, “he was starting to masturbate with heterosexual fantasies, but he expressed the following difficulty which was never completely overcome… ‘whenver I start to think of the vagina a penis comes into my mind — as though there was some kind of block.’ Treatment stopped after 39 sessions. Although he had started to find women attractive and to masturbate with heterosexual fantasies for the first time in his life, his homosexual interest had never been significantly reduced and had remained prepotent. … After four months homosexual urges became stronger and heterosexual fantasies difficult. After 6 months he resumed homosexual activities. Soon he was back to his normal pattern.”
Patient C: A 37-year-old zoologist who volunteered because “he wanted to become heterosexual.”After 12 sessions he was experiencing ‘pangs’ of anxiety on seeing attractive males in the street. By this stage he was beginning to masturbate with heterosexual fantasies. After 15 sessions he started to feel some anxiety during the female trials and a little later was noting ‘pangs’ of anxiety on seeing sexually threatening females as well as attractive males. This conditioned anxiety became more obvious and treatment was stopped after 35 sessions… For 2½ years he has maintained this conditioned ‘phobic’ anxiety to potentially attractive males, experiencing a ‘pang’ of discomfort in the chest when seeing them. On two or three occasions homosexual advances have been made to him and these have provoked intense anxiety and avoidance. …Two and a half years after treatment his homosexual interest is much reduced and he has no desire to make any homosexual contacts. He is once again using homosexual fantasies during masturbation but heterosexual fantasies occur some of the time.”
Patient D: A 22-year-old “with no settled employment, with an abnormal personality … [and who] also suffered from epilepsy.” “He showed inconsistent and varied responses during treatment and was an unreliable witness. There was slight improvement in the first half of treatment but the second half resulted in a hostile, negativistic and destructive attitude together with some depression of mood. He made a suicidal gesture and his first ever homosexual advance during this stage. Treatment was stopped after 36 sessions with no apparent benefit having been achieved.” After treatment, “he appeared much more accepting of his homosexuality.” But his sexual functioning was disturbed, possibly because of the effects of treatment: “He found little pleasure and was unable to reach orgasm. Nine months after treatment he was playing a passive role in buggery, but with no sexual arousal on his part. Two years after treatment he was much more settled and was having an affair with an elderly man in which sexual activity was getting less and less frequent. He still failed to achieve orgasm during these encounters…”
Patient E: A 36-year-old actor “of athletic build.” Despite heing “actively homosexual,” he met and married a woman and subsequently became “almost impotent,” and for the year before undergoing treatment, he had been suffering from “intrusive homosexual fantasies [which] were still strong and frequent” along with “marked pervasive anxiety.” After 12 sessions, he began having intercourse with his wife “with slight enjoyment.” But after 32 sessions, “both heterosexual and homosexual responses were declining again. At this stage, homosexual fantasies provoked disinterest rather than anxiety, whereas heterosexual fantasies, especially involving his wife, provoked some anxiety.” On follow-up things only got worse. “Ten months after treatment, his relationship with his wife deteriorated again, his anxiety increased and he became completely imporent. One month later homosexual fantasies returned. He expressed anger at the treatment and the therapist and discontinued treatment.”
Patient F: A 47-year-old Scot who sought treatment for many years to become heterosexual. He had previously tried psychotherapy (including psychotherapy with LSD), and two previous, unsuccessful attempts at electric shock aversion therapy. So this was a guy who knew what he was getting into. “He reported relief at the start of female trials after only 2 sessions. After 8 sessions he started to produce strong erections to heterosexual fantasies. From then on the pattern was of fluctuating heterosexual interest. Homosexual interest and responses were reduced early in treatment, but showed a slight increase in the second half. Treatment was stopped after 35 sessions. At this stage he felt ‘really heterosexual now’ and had only occasional slight homosexual interest.” But his “really heterosexual” feelings proved elusive. He dated a woman, but when they broke up he was depressed for two to three weeks and “his homosexual interest increased and he had two homosexual experiences. Fifteen months after treatment, following a second severe but short lived depressive episode he is showing more homosexual interest again, but retains some heterosexual interest and has certainly not regained his previous ‘heterophobia’.”
Patient G: A 27-year-old clerical worker who had almost no heterosexual experience or feelings. “After 9 sessions he was finding heterosexual fantasies easier and after 12 sessions he was reporting an intense interest in women. Though fluctuating in intensity, heterosexual responses and interest continued for the rest of treatment. His homosexual interest and responses were slightly reduced during the middle stages of treatment but after 17 sessions they increased again. Treatment was stopped after 32 sessions, when his homosexual interest was much the same as before treatment, but he now found women strongly attractive.”
“Following treatment he became depressed, his homosexual urges became more marked and his heterosexual interest lessened. He remained depressed for the next five months. Then, following a minor rejection by a homosexual friend, he was admitted to hospital having been found wandering the streets at night removing some of his clothing. He showed no further evidence of psychotic behaviour. For the first month in hospital he remained isolated and mildly depressed. He was then started on diazepam and showed a marked change. He became more cheerful and confident and started a relationship with a female patient which continued after they both left hospital. At first he showed some degree of impotence, but he has had a satisfactory sexual relationship with her since. Fifteen months after aversion he enjoys regular sexual intercourse and has had no homosexual inclinations at all.
Patient H: A 24-year-old teacher who, despite strong attractions, had had little homosexual experience. While had had had several girlfriends, he found them “only slightly arousing.” “After 7 sessions he started to produce increasingly strong heterosexual responses associated with aggressive fantasies. After 15 sessions heterosexual images were beginning to intrude into his homosexual masturbation fantasies and a little later he masturbated with exclusively heterosexual fantasies for the first time. By this stage his homosexual interest was less strong and he had become unable to reach orgasm using homosexual fantasies. His homosexual responses in treatment continued as strong, however.” Following treatment, he began dating a girl, but the relationship never progressed beyond kissing. It ended after three months. “Six months after treatment, he made his first homosexual contact. One year after treatment he is energetically pursuing homosexual relationships but he avoids reaching orgasm himself, and if possible prevents his partner from doing so.”
Patient I: A 29-year-old policeman, married since 21, and with two children. When he first married, he “obtained slight pleasure from sexual intercourse but this steadily waned.” He began a three year affair with another man “and is not promiscuous,” during which time he became “mostly impotent with his wife.” He volunteered for treatment to try to save his marriage, but the treatment proved futile. “Little impression was made on either his homosexual or heterosexual responses. There was some reduction in homosexual urges after 5 sessions but he avoided using his ‘affair’ in his homosexual fantasies and was clearly resisting any attempt to destroy his feelings for him. He reported little anxiety during treatment but he was generally non-communicative and difficult to assess. After 20 sessions the treatment was changed to Method B. He was urged to use fantasies involving his ‘affair’. After only one further session it became clear that he did not really want the treatment to work. The treatment was therefore discontinued.” On follow-up, “he returned to his previous homosexual relationship with considerable pleasure and continued a reasonably friendly though sexless relationship with his wife.”
Patient J: A 27-year-old “of average intelligence” who, while never having had any heterosexual interest, he “could never contemplate an overt homosexual relationship because of guilt.” “He had 15 sessions of method A and 15 sessions of Method B. His responses were inconsistent. During Method A he was usually unable to concentrate on his fantasies for fear of the shock, even when very low levels were used. Occasionally, however, he responded easily. With Method B the same inconsistency occurred. At the end of treatment there was no evidence of change in his homosexuality, and the only change heterosexually was that he had lost his revulsion and was now able to sustain heterosexual fantasies more easily. … “In the first three months (after treatment), he experienced more interest in females. He mixed more with them socially, and kissed a girl for the first time. This did not, however, result in any sexual arousal. His homosexual fantasies continued as strongly as before. Ten months after treatment there is no further progress.
As you can see, there were precious few success stories — and you would have to find some rather expansive definition of “success” to find them. Patient G, according to Bancroft, was the only one to show “no homosexual inclinations at all.” But one has to wonder what priced he paid. Later in the article, Patient G was among four who showed moderate or high anxiety during treatment, and he “expressed some slight aggression toward the therapist on 3 or 4 occasions.” He also “became depressed soon after treatment and remained so, in spite of anti-depressant drugs, until admission to hospital 5 months later.” Bancroft attributed his subsequent improvement not to his lady friend, but to the use of Diazepam.
Overall, Bancroft found the results disappointing, but he felt it was important to press on:
Methods of behaviour modification such as these are in their infancy and a considerable amount of further research is needed before such techniques can be advocated for general use. But the benefits to be gained from such research may be considerable. They will include increased understanding of behaviour modification in general, as well as a greater understanding of the behaviours to be modified.
The Rest Of The Story
I would love to know what happened to those ten patients since their treatment ended in the mid-1960s, but nearly fifty years on we may never find out. But we do know that Bancroft would continue investigating methods for changing sexual orientation through the 1960s and the first part of the 1970s. But as the mental health professions changed its view of homosexuality, and as behavior therapists in particular began to abandon their punitive approaches to behavioral modification, Bancroft tried to move with the times, although he did so reluctantly. In 1975 — by then he was Dr. John Bancroft at the Department of Psychiatry at Oxford University — he wrote the following:
I accept that homosexuality is not an illness but an alternative sexual life style which may be and often is compatible with normal health, and with those interpersonal and social values that we hold most high. If that is so then the social stigma associated with homosexuality, the repression that stems from it and the guilt and suffering that often result are undesirable and unjust. When we consider the part that the medical profession has played in the past in fostering these negative and unjust social attitudes it is clear that it has a responsibility now and in the future actively to encourage a more positive and less repressive climate of opinion.
Good start, right? But the balance of his 1975 article was somewhat more ambivalent. He defended aversion therapy against those who denounced its coercive nature, considering it little more than a public relations problem. He defended therapies — including aversion therapies — to change sexual orientation if a patient said he wanted it. “Homosexuals are subjected to many types of oppression: one of the most hostile can be the attitude, ‘You are a homosexual — you must learn to accept it’.”
But in the decades since, Bancroft has had the occasion to reconsider that position further. When Robert Spitzer published his controversial ex-gay study in the Archives of Sexual Behavior in 2003 (the study that Spitzer renounced and later apologized for earlier this year), Bancroft, now at the Kinsey Institute for Research in Sex, Gender, and Reproduction at Indiana University, was one of some two dozen authors to publish a peer review commentary. In Bancroft’s response, he drew on his own experience in the field:
Times were different then. The Gay Rights Movement was early in its development and it was much more likely than it is today that individuals would seek such change. But on reflection, I realized that, whereas I was genuinely trying to help the individual, in the process I was aligning myself with those who reinforced homophobic attitudes and all the consequences of the stigma that ensued. It did not continue to be a dilemma for me, as my own results gave me no reason to continue to use such simplistic interventions.
And he criticized Spitzer’s study claiming that some people who underwent “reparative” therapy said they changed. He criticized it not only for its many methodological weaknesses, but also for the role it would inevitably play in reinforcing negative attitudes toward gay people:
If there were any grounds for regarding homosexual orientation as a pathology rather than a variant of human sexual expression, then treating the pathology might be justified. I would assert that there are no such grounds, and hence providing treatment on that basis is professionally unethical and, according to my value system, immoral. There is a long and disturbing history of medical practitioners imposing their moral values through their professional practice. The imposition of moral values, explicitly or implicitly, that is, urging someone to undergo change because their current sexual orientation is immoral, should not be regarded as “therapy,” and in any case raises other ethical and moral issues. …[Spitzer’s report] constitutes vigorous reinforcement of homophobia and the social stigma experienced by those with homosexual identities in our society. Together, this results
in widespread suffering for homosexual minorities and, no doubt, for many who are pressured into attempting such change, considerable conflict and unhappiness.
[Sources: John Bancroft. “Aversion therapy of homosexuality: A pilot study of 10 cases.” British Journal of Psychiatry 115, no. 529 (December 1969): 1417-1431.
John Bancroft. “Homosexuality and the medical profession: A behviourist’s view.” Journal of Medical Ethics 1, no. 4 (December 1975): 176-180.
John Bancroft. Peer Comments on Spitzer (2003): “Can sexual orientation change? A long-running saga.” Archives of Sexual Behavior 32, no. 5 (October 2003): 419-421.
For more information on the history of behavioral therapy, see our report, “Blind Man’s Bluff”.]
If you know of something that belongs on the Agenda, please send it here. Don’t forget to include the basics: who, what, when, where, and URL (if available).
As always, please consider this your open thread for the day.
Latest Posts
Featured Reports
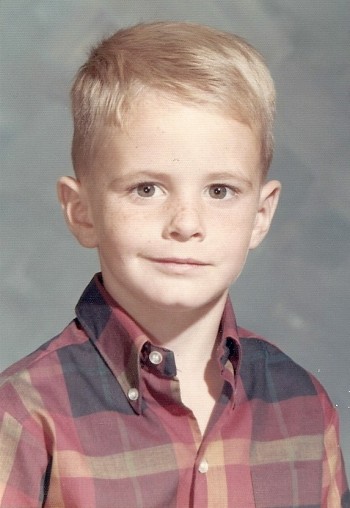 In this original BTB Investigation, we unveil the tragic story of Kirk Murphy, a four-year-old boy who was treated for “cross-gender disturbance” in 1970 by a young grad student by the name of George Rekers. This story is a stark reminder that there are severe and damaging consequences when therapists try to ensure that boys will be boys.
In this original BTB Investigation, we unveil the tragic story of Kirk Murphy, a four-year-old boy who was treated for “cross-gender disturbance” in 1970 by a young grad student by the name of George Rekers. This story is a stark reminder that there are severe and damaging consequences when therapists try to ensure that boys will be boys.
When we first reported on three American anti-gay activists traveling to Kampala for a three-day conference, we had no idea that it would be the first report of a long string of events leading to a proposal to institute the death penalty for LGBT people. But that is exactly what happened. In this report, we review our collection of more than 500 posts to tell the story of one nation’s embrace of hatred toward gay people. This report will be updated continuously as events continue to unfold. Check here for the latest updates.
In 2005, the Southern Poverty Law Center wrote that “[Paul] Cameron’s ‘science’ echoes Nazi Germany.” What the SPLC didn”t know was Cameron doesn’t just “echo” Nazi Germany. He quoted extensively from one of the Final Solution’s architects. This puts his fascination with quarantines, mandatory tattoos, and extermination being a “plausible idea” in a whole new and deeply disturbing light.
On February 10, I attended an all-day “Love Won Out” ex-gay conference in Phoenix, put on by Focus on the Family and Exodus International. In this series of reports, I talk about what I learned there: the people who go to these conferences, the things that they hear, and what this all means for them, their families and for the rest of us.
Prologue: Why I Went To “Love Won Out”
Part 1: What’s Love Got To Do With It?
Part 2: Parents Struggle With “No Exceptions”
Part 3: A Whole New Dialect
Part 4: It Depends On How The Meaning of the Word "Change" Changes
Part 5: A Candid Explanation For "Change"
 At last, the truth can now be told.
At last, the truth can now be told.
Using the same research methods employed by most anti-gay political pressure groups, we examine the statistics and the case studies that dispel many of the myths about heterosexuality. Download your copy today!
And don‘t miss our companion report, How To Write An Anti-Gay Tract In Fifteen Easy Steps.
 Anti-gay activists often charge that gay men and women pose a threat to children. In this report, we explore the supposed connection between homosexuality and child sexual abuse, the conclusions reached by the most knowledgeable professionals in the field, and how anti-gay activists continue to ignore their findings. This has tremendous consequences, not just for gay men and women, but more importantly for the safety of all our children.
Anti-gay activists often charge that gay men and women pose a threat to children. In this report, we explore the supposed connection between homosexuality and child sexual abuse, the conclusions reached by the most knowledgeable professionals in the field, and how anti-gay activists continue to ignore their findings. This has tremendous consequences, not just for gay men and women, but more importantly for the safety of all our children.
Anti-gay activists often cite the “Dutch Study” to claim that gay unions last only about 1½ years and that the these men have an average of eight additional partners per year outside of their steady relationship. In this report, we will take you step by step into the study to see whether the claims are true.
Tony Perkins’ Family Research Council submitted an Amicus Brief to the Maryland Court of Appeals as that court prepared to consider the issue of gay marriage. We examine just one small section of that brief to reveal the junk science and fraudulent claims of the Family “Research” Council.
 The FBI’s annual Hate Crime Statistics aren’t as complete as they ought to be, and their report for 2004 was no exception. In fact, their most recent report has quite a few glaring holes. Holes big enough for Daniel Fetty to fall through.
The FBI’s annual Hate Crime Statistics aren’t as complete as they ought to be, and their report for 2004 was no exception. In fact, their most recent report has quite a few glaring holes. Holes big enough for Daniel Fetty to fall through.
Ben in Oakland
December 8th, 2012
So the grand inquisitor finally realized that he was not really behaving like a Christian.
Whoopsie? Did I venture into the wrong narrative?
John D
December 10th, 2012
Oil lasting for eight days? That is so not the real story of Hanukkah.
Hanukkah is eight days long because the Maccabees promised their followers that they would have control of the Temple by Sukkot (which is eight days long). When they failed to do so, they held a late Sukkot as part of rededicating (hanukkah) the Temple. The miracle stories come much later.
Leave A Comment