Box Turtle Bulletin
 News and commentary about the anti-gay lobby
News and commentary about the anti-gay lobby News and commentary about the anti-gay lobby
News and commentary about the anti-gay lobbyAugust 9th, 2012
Yesterday, I posted a video interview of Dr. Paul Semugoma (many of you know him as GayUganda) talking about the challenges of confronting HIV/AIDS in a country with such rampant homophobia that it is dangerous for LGBT people to disclose themselves to their doctors. Dr. Semugoma also spoke at a plenary session at the International AIDS Conference in Washington D.C. on July 27, discussing “The Dynamics of the Epidemic in Context,” the particular context being that in many governments around the world are unwilling to address the reality that gay men exist in their countries.
In addition to the video above, you can find an error-laden transcript of his talk here(PDF: 160KB/55 pages). While Dr. Semoguma had come out in Facebook and other social media, this was his coming-out moment, quite literally, on the world stage (at about the 3:15 mark):
Men who have sex exist with men, everywhere. You know, it’s kind of interesting to start like that. When we talk about men who have sex with men, actually I am also a man who has sex with men. [applause.] It’s a major and important point to point out that men who have sex with men exist everywhere. If we say that they don’t exist then we don’t know how to deal with them, we don’t know how to get to the challenges that we have in HIV prevention with them.
He then described a pivotal moment in his life which showed him that the epidemic would never be dealt with successfully unless gay and bisexual men are included in HIV-prevention messages (at about the 4:35 mark):
I want to tell you a story about the patient who changed my life. This was in 2004. I was by then a medical doctor. I had studied in two medical schools, that is at Muhimbili Medical Center in the University of Dar es Salaam and I had also studied at Makerere University. I had a bit of work up country, and then I’d gone back to Kampala, which is the capital city of Uganda, to start work in private practice.
As I said, I’m a gay man. I had been dealing with HIV amongst Ugandans and I knew it was a disease that is spread by sex, but I had not been confronted by then by the fact that HIV is also spread by gay sex. I didn’t have that link. So I was faced by this guy. He was gay. I knew him. He had bisexual practices meaning he used to sleep with men and at some point in time he had slept with women. And He had been recently diagnosed with HIV.
One of the things that he told me was, “One of my lovers must have slept with a woman.” I was like, “You didn’t sleep with a woman at this particular point, you must have got it from your lover.” But his point was since I’ve been seeing all these nice photos of men and women and the government telling us, “Be careful, love carefully.” These are the ones who spread HIV; it is the women who give it to us. But he also asked me a question: how do I protect my lovers? And that was the question that changed my life. I knew at that particular moment that I didn’t know how to protect him, how to give him the information, how to tell him to protect his lovers, and that was the changing point because I then discovered that because I didn’t know, I was ignorant. I was in sort of denial because I was a gay man and I am still a gay man. I just needed to know.
I had access to the internet and I quickly educated myself, something which we all have to do. It is important that we leave from being just friendly to MSM, to men who have sex with men, to being competent in care. [applause]
This ignorance and denial it didn’t happen just with me. It is also with everybody. Just a few months ago, about three months ago in Uganda the first LGBT clinic was opened by one of the groups, one of the LGBT groups. They were saying that, well, we do not have a clinic, the doctors don’t really know the problems that we have and we need a clinic. They got funding (very good) put the clinic in Kampala (very good) and then made sure that the government
didn’t know.Then, what touched me was that three doctors were asked in Uganda. “What do you think about this?” They were saying, “We do not discriminate because we are doctors,” which is fantastic. Then, they said, “We do not discriminate because we do not ask about sexual orientation.” Now, if you do not ask about sexual orientation then that means that you are not aware that men who
have sex with men actually come and sit with you in the consultation room, and that men who have sex with men actually have a higher risk of HIV. [ applause]This ignorance is part of what is there. We have to ask ourselves the question. Are we going to an AIDS-free generation without including MSM? Actually the answer from the science that we have is that no, we are not going to do that.
Dr. Semugoma then gave an overview of the populations most at risk, including not only gay men, but also within the gay community, black gay men. And he also discussed the general problems of reaching “pariah” communities in different countries, including here in the U.S., Canada, and Britain. He then returned his attention back to Africa and the structural barrier that those of us who have been following events in Uganda are all too aware of: criminalization (at about the 15:00 mark):
Criminalization. I have heard this over and over again. You are dealing with a criminal population and the criminal population somehow seems to not be citizens, somehow seem not to fit to have intervention, somehow they just don’t seem to deserve the attention that others get even in HIV prevention.
This is the relationship between criminalization and sex practices. Untargeted expenditure. This is for HIV programming. We saw that HIV burden is actually higher amongst MSM but what actually happens when the monies for HIV
prevention go to the countries there’s attenuation. Less and less gets to the MSM because of the stigma, because they are criminals.…This case study is of Senegal. Senegal is a country in West Africa has an epidemic which is concentrated amongst MSM. They actually were one of the first African countries to do an MSM-targeted HIV prevention effort. They did a study, which I was very happy to come across in 2004. They saw that they have a concentrated epidemic with HIV 20 times higher amongst the MSM than in the general population. They did comprehensive outreach in place for MSM.
In 2008, we had this ICASA, ICASA is the equivalent of AIDS meeting for Africa. During that ICASA, they actually came to tell the rest of the country about what was happening that they are doing some HIV prevention amongst the highest risk population in Senegal. After ICASA, nine outreach workers were arrested and prosecuted. They were released April 2009. They had been convicted of spreading homosexuality most likely. The issue was that happening actually almost destroyed the HIV outreach amongst the highest risk population in Senegal.
Now, let’s talk about my country, Uganda. Uganda had a study done in 2008, a study done in Kampala. The HIV rate was almost 14 percent, but it’s 13.7 percent amongst MSM in Kampala, compared to a rate of 4.4-percent amongst other men in Kampala, which actually means that this was a high-risk population. During the time of the study the Director General of Uganda AIDS, the national program, said that for the first time he actually admitted that MSM exists in Uganda — which was a positive — but he said we are not going to deal with them.
Now, what happened is that some of us decided that no, this was a bit too much and we had the Implementers’ Meeting happening in Uganda, and we decided to come and storm the meeting and held a five minute protest. What happened after that was that some of us were arrested and they continued to be prosecuted for demanding for HIV prevention program amongst MSM in Uganda. For demanding for an HIV prevention program amongst a vulnerable population in Uganda. That’s why there were prosecuted.
Now, this had an effect on the study which was happening in Kampala at that time. Those people were studying the respondents, that MSM were not coming to the study, the respondents who are not coming. The recruitment dipped, it recovered sometime later, but then dipped again, because Uganda unfortunately is a very highly homophobic country. They got about 300 respondents, which in six months was very few homosexuals, compared to Kenya, compared to Tanzania, compared to Zanzibar. In two months they’ll get 500 people. In the first study in Kenya they actually had to stop the study, because in Nairobi they were getting more than 500 gay people.
Now, Uganda has definitely been one of the worst offenders in HIV prevention for MSM. They want to ban the agencies which work for gay rights. That was about last month I think. And the LGBT clinic, it needs to be shut. All this homophobia is actually happening when we have a study done with folks that we have a vulnerable population, which actually is responding to the homophobia in the country. Okay, HIV prevalence amongst the MSM was related to external homophobia.
Dr. Semugoma ended his talk with a stirring call to action, which hinged on increased visibility of gay men and the elimination of homophobia, anti-AIDS stigma, and ignorance about HIB/AIDS. He also remembered that the advocacy fights to achieve those aims are not without cost (at the 26:30 mark):
Now, I wanted to acknowledge the fact that a lot of people have helped me to prepare this speech, but I remembered that I can acknowledge also those people who have lost this fight, I mean who have been killed, the price of advocacy. Advocates are beaten, they are arrested, they are killed. I just wanted to remember these few, Alim Mongoche in Cameroon; Steve Harvey in Jamaica, David Kato in Uganda, Thapelo Makutle in South Africa [applause].
One of my most enduring memories of David Kato is of him when we went into the Implementers’ Meeting when he wanted to engage the speakers, and then running very fast on this big road with the police behind him. They wanted to arrest him because we had barnstormed the Implementers’ Meeting.
Many stories are untold and unreported. It is tough to achieve comprehensive HIV prevention and treatment in this context, but it has been done. It has been done before. It is being done now. It is going to be done again. We have tried and they continue to try.
At the end of his talk, he acknowledged his partner, whose name I did not catch. But it was very heartwarming to see him lean into the microphone and say, out loud, “I love you.”
Latest Posts
Featured Reports
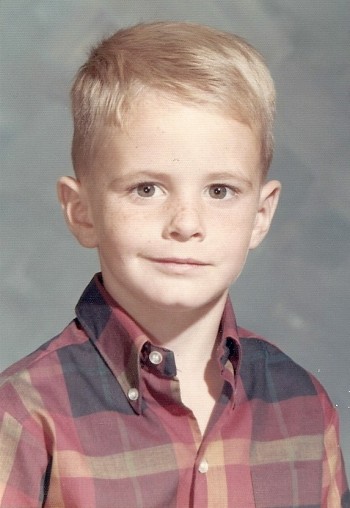 In this original BTB Investigation, we unveil the tragic story of Kirk Murphy, a four-year-old boy who was treated for “cross-gender disturbance” in 1970 by a young grad student by the name of George Rekers. This story is a stark reminder that there are severe and damaging consequences when therapists try to ensure that boys will be boys.
In this original BTB Investigation, we unveil the tragic story of Kirk Murphy, a four-year-old boy who was treated for “cross-gender disturbance” in 1970 by a young grad student by the name of George Rekers. This story is a stark reminder that there are severe and damaging consequences when therapists try to ensure that boys will be boys.
When we first reported on three American anti-gay activists traveling to Kampala for a three-day conference, we had no idea that it would be the first report of a long string of events leading to a proposal to institute the death penalty for LGBT people. But that is exactly what happened. In this report, we review our collection of more than 500 posts to tell the story of one nation’s embrace of hatred toward gay people. This report will be updated continuously as events continue to unfold. Check here for the latest updates.
In 2005, the Southern Poverty Law Center wrote that “[Paul] Cameron’s ‘science’ echoes Nazi Germany.” What the SPLC didn”t know was Cameron doesn’t just “echo” Nazi Germany. He quoted extensively from one of the Final Solution’s architects. This puts his fascination with quarantines, mandatory tattoos, and extermination being a “plausible idea” in a whole new and deeply disturbing light.
On February 10, I attended an all-day “Love Won Out” ex-gay conference in Phoenix, put on by Focus on the Family and Exodus International. In this series of reports, I talk about what I learned there: the people who go to these conferences, the things that they hear, and what this all means for them, their families and for the rest of us.
Prologue: Why I Went To “Love Won Out”
Part 1: What’s Love Got To Do With It?
Part 2: Parents Struggle With “No Exceptions”
Part 3: A Whole New Dialect
Part 4: It Depends On How The Meaning of the Word "Change" Changes
Part 5: A Candid Explanation For "Change"
 At last, the truth can now be told.
At last, the truth can now be told.
Using the same research methods employed by most anti-gay political pressure groups, we examine the statistics and the case studies that dispel many of the myths about heterosexuality. Download your copy today!
And don‘t miss our companion report, How To Write An Anti-Gay Tract In Fifteen Easy Steps.
 Anti-gay activists often charge that gay men and women pose a threat to children. In this report, we explore the supposed connection between homosexuality and child sexual abuse, the conclusions reached by the most knowledgeable professionals in the field, and how anti-gay activists continue to ignore their findings. This has tremendous consequences, not just for gay men and women, but more importantly for the safety of all our children.
Anti-gay activists often charge that gay men and women pose a threat to children. In this report, we explore the supposed connection between homosexuality and child sexual abuse, the conclusions reached by the most knowledgeable professionals in the field, and how anti-gay activists continue to ignore their findings. This has tremendous consequences, not just for gay men and women, but more importantly for the safety of all our children.
Anti-gay activists often cite the “Dutch Study” to claim that gay unions last only about 1½ years and that the these men have an average of eight additional partners per year outside of their steady relationship. In this report, we will take you step by step into the study to see whether the claims are true.
Tony Perkins’ Family Research Council submitted an Amicus Brief to the Maryland Court of Appeals as that court prepared to consider the issue of gay marriage. We examine just one small section of that brief to reveal the junk science and fraudulent claims of the Family “Research” Council.
 The FBI’s annual Hate Crime Statistics aren’t as complete as they ought to be, and their report for 2004 was no exception. In fact, their most recent report has quite a few glaring holes. Holes big enough for Daniel Fetty to fall through.
The FBI’s annual Hate Crime Statistics aren’t as complete as they ought to be, and their report for 2004 was no exception. In fact, their most recent report has quite a few glaring holes. Holes big enough for Daniel Fetty to fall through.
F Young
August 9th, 2012
According to Jim Pickett of the Windy City Times, Paul’s partner is Brian Kanyemba, who is now a research assistant at the Desmond Tutu HIV Foundation in Cape Town.
They have their photo here: http://www.windycitymediagroup.com/lgbt/AIDS-2012-And-Lube/38841.html
Darina
August 9th, 2012
Thank you, Jim. I’m in awe of Dr. Semugoma.
charmonium
August 11th, 2012
Thanks for the link. He’s an amazing man. For those who want to see the slides he’s talking about, there’s a link to the powerpoint on this page. http://pag.aids2012.org/session.aspx?s=677
Leave A Comment